Subtitle: Mastering Minimally Invasive Approaches in Contemporary Aesthetic Prosthodontics
Target Keywords: direct composite veneers, aesthetic prosthodontics, minimally invasive dentistry, composite layering technique, smile design, composite polishing protocols, digital smile planning, anterior restorations
Executive Summary
This comprehensive article addresses the renaissance of direct composite veneers as a sophisticated, minimally invasive treatment modality in contemporary aesthetic prosthodontics. While indirect ceramic restorations have dominated aesthetic dentistry discourse, advanced composite materials and refined application techniques have positioned direct composite veneers as a clinically superior option for carefully selected cases. The article examines current evidence on case selection parameters, preparation designs, layering protocols, and finishing techniques that maximize aesthetic outcomes while preserving tooth structure. Recent advances in composite formulations have resolved historical limitations regarding wear resistance, color stability, and polishability, with contemporary nanohybrid and nanofilled materials demonstrating 5-year survival rates exceeding 85% according to the latest clinical studies. Digital planning advancements including 3D-printed mock-ups and predictive software have transformed the diagnostic phase, enabling precise communication and predictable outcomes. Through detailed case studies spanning diverse clinical scenarios—from diastema closure to tetracycline discoloration management—this article provides practitioners with actionable protocols for incorporating direct composite veneers into their aesthetic armamentarium. Special focus is placed on emerging techniques including injection molding, stamp techniques, and biomimetic layering approaches. For clinicians seeking to expand their minimally invasive treatment options while achieving exceptional aesthetics, this article provides evidence-based guidelines for patient selection, material choice, technical execution, and long-term maintenance of direct composite veneers.
1. Introduction & Background
The pursuit of minimally invasive approaches represents one of the most significant paradigm shifts in restorative and aesthetic dentistry over the past decade. Direct composite veneers embody this philosophy, offering preservation of tooth structure while providing remarkable aesthetic improvements when properly executed. Despite the dominance of ceramic materials in high-end cosmetic dentistry, contemporary direct composite systems have undergone revolutionary advancements in physical properties, handling characteristics, and optical behavior.
Historical reluctance toward direct composites for anterior aesthetics stemmed from legitimate concerns regarding wear resistance, color stability, and polishability. However, modern nanohybrid and nanofilled composites have dramatically narrowed the performance gap with ceramics. Studies by Peumans et al. (2022) report 5-year survival rates of 89.4% for direct composite veneers, challenging the notion that these restorations should be considered merely “provisional” or “compromised” alternatives to porcelain.
The economic landscape of dentistry further emphasizes the relevance of direct composite veneers. Patient financial constraints, coupled with growing interest in conservative approaches, have created an environment where cost-effective, minimally invasive solutions are increasingly sought after. Direct composite veneers typically cost 40-60% less than their ceramic counterparts while offering immediate results without laboratory dependencies.
Technological integration has further elevated direct composite procedures. Digital smile design, 3D-printed mockups, and silicone indices derived from virtual wax-ups have transformed the diagnostic and treatment planning phases. These technologies enable precise communication with patients and predictable transfer of planned aesthetics to the final restorations.
This article aims to provide clinicians with evidence-based protocols for case selection, material choice, preparation design, application techniques, and maintenance strategies for direct composite veneers. By mastering these procedures, practitioners can expand their conservative treatment options while achieving aesthetic outcomes that satisfy even the most discerning patients.
2. Clinical/Technical Overview
Nanofilled Composites

- Particle size: 20-75nm
- Superior polish retention with average gloss retention of 85% after 5,000 toothbrush cycles
- Higher translucency (15-25%) appropriate for incisal effects
- Examples: 3M Filtek Supreme Ultra, Tokuyama Estelite Omega
Nanohybrid Composites

- Combined nanofiller (40-50nm) with microfillers (0.1-2μm)
- Balanced opacity (65-85%) ideal for dentin replacement
- Enhanced mechanical properties (flexural strength 120-150 MPa)
- Examples: GC G-ænial, Coltene Brilliant EverGlow
Injectable Composites
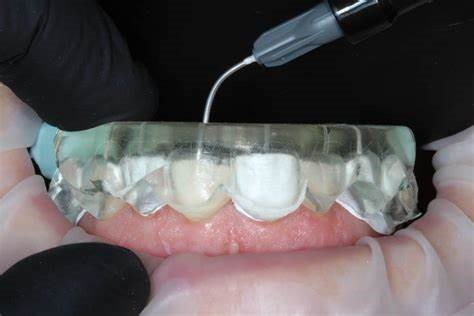
- Flowable consistency with high filler loading (65-70% by weight)
- Reduced polymerization shrinkage (1.8-2.4%)
- Precise delivery for complex morphology replication
- Examples: GC G-ænial Universal Injectable, Estelite Universal Flow
Microhybrid Composites

- Traditional formulations with proven long-term performance
- Average particle size 0.4-1.0μm
- Higher chameleon effect for shade integration
- Examples: Voco Grandio, Ivoclar Tetric EvoCeram
The clinical decision framework for material selection depends on several factors:
| Clinical Scenario | Recommended Composite Type | Primary Rationale |
| Minimal discoloration | Nanofilled | Higher translucency for blending |
| Moderate-severe discoloration | Nanohybrid | Better masking capability |
| Significant build-up (>2mm) | Microhybrid | Enhanced mechanical properties |
| Diastema closure | Injectable | Precise margin adaptation |
| Multi-unit cases | Layer-specific systems | Optical depth and characterization |
B. Preparation Designs for Direct Composite Veneers
Unlike ceramic veneers requiring standardized preparation, direct composite veneers employ case-specific preparation designs based on clinical needs:
No-Preparation Approach
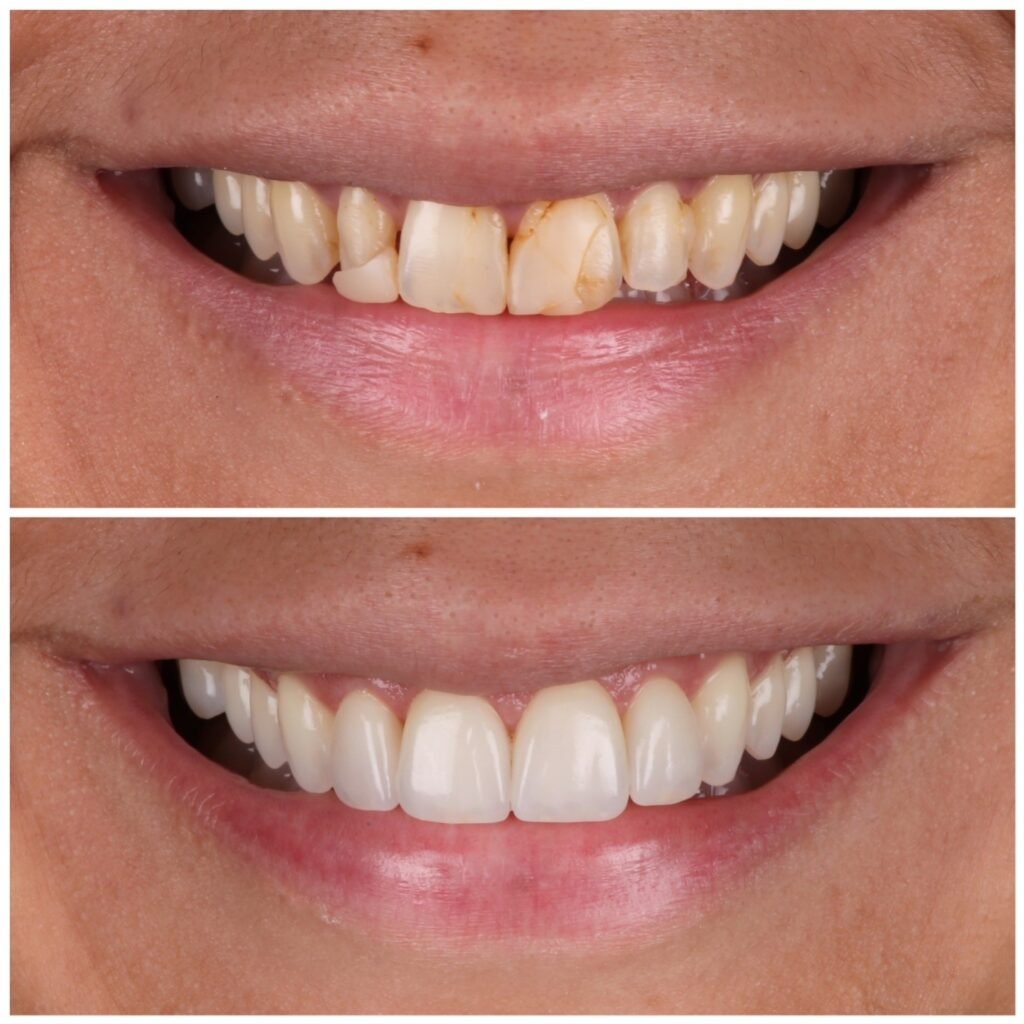
- Indication: Minor shape corrections, small diastemas
- Protocol: Microroughening with 50μm aluminum oxide, phosphoric acid etching
- Advantage: Complete preservation of enamel structure
- Limitation: Limited ability to mask discoloration
Minimally Invasive Preparation
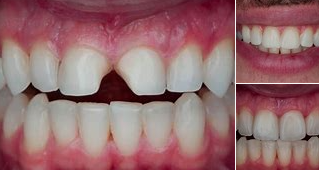
- Indication: Moderate discoloration, minor alignment correction
- Protocol: 0.3-0.5mm facial reduction, supragingival margins, preservation of proximal contacts
- Advantage: Maintains 95%+ of tooth structure while enabling shade modification
- Limitation: Requires precise depth control
Veneer-Wrap Preparation
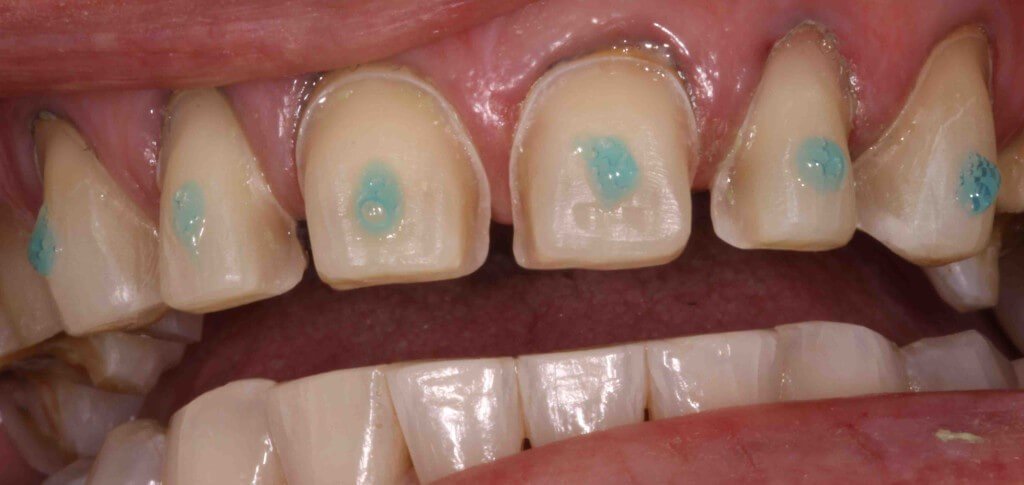
- Indication: Significant shape correction, moderate crowding
- Protocol: Facial reduction (0.5-0.7mm), proximal extension to contact areas
- Advantage: Greater control over emergence profile and proximal contours
- Limitation: More technically demanding, higher risk of overcontouring
Research by LeSage (2021) demonstrated that preserving the enamel-dentin junction in direct veneer preparations significantly enhances bond strength (32% higher μTBS values) compared to preparations extending into dentin. This preservation should be prioritized whenever possible.
C. Layering Techniques and Application Protocols
The application technique selected dramatically influences the aesthetic outcome and efficiency of the procedure:
Polychromatic Layering (Traditional)
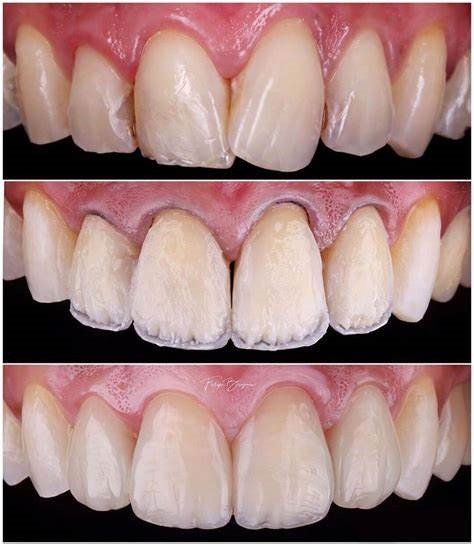
- Distinct layers of dentin, enamel, and effect shades
- 3-5 separate increments per veneer
- Highly customized optical effects possible
- Technique-sensitive with longer chairtime
Dual-Layer Approach (Simplified)
- Two primary layers: dentin core (higher opacity) and enamel layer (higher translucency)
- Balance between efficiency and aesthetics
- 85% of cases can achieve excellent results with this approach
Monolayer Technique
- Single shade of body/universal material
- Suitable for minimal corrections with high shade integration needs
- Most efficient but limited aesthetic control
Injection Molding Technique
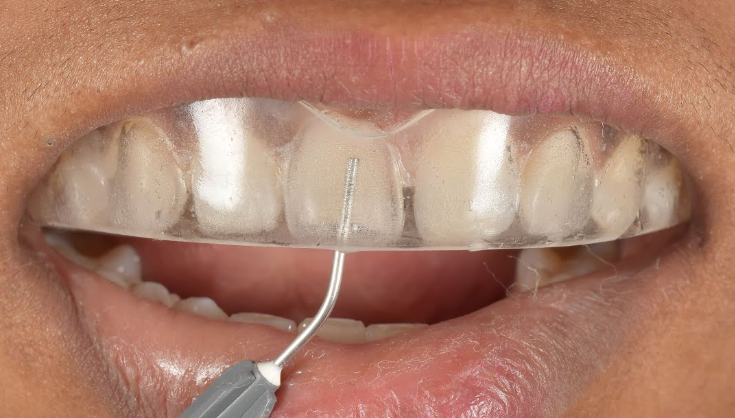
- Utilizes silicon index derived from wax-up
- Injectable composite delivered under pressure
- High precision for multiple-unit cases
- Reduced air incorporation and handling variables
Stamp Technique
- Index records pre-operative or wax-up surface anatomy
- Direct impression of final anatomy transferred to composite
- Minimal finishing required
- Excellent for fractured tooth restoration or replacement of existing restorations
Recent clinical trials by Dietschi et al. (2023) found that the simplified dual-layer approach achieved aesthetic scores statistically comparable to the more complex polychromatic technique in 87% of cases, while reducing chairtime by an average of 24 minutes per case.
3. Case Studies & Clinical Applications
Case Study 1: Diastema Closure with No-Prep Approach
Patient Profile:
- 28-year-old female
- Chief complaint: Multiple anterior diastemas affecting smile confidence
- Clinical findings: 1.5mm diastema between #8-9, 0.8mm spaces between #7-8 and #9-10
- Excellent oral hygiene, no caries, minimal to no discoloration
Treatment Approach:
- Digital smile design and 3D-printed mock-up for patient approval
- Creation of silicone palatal index from approved mock-up
- Isolation with rubber dam and sectional matrix system
- Surface preparation: prophylaxis with pumice, air abrasion (50μm aluminum oxide), phosphoric acid etching (37%, 30 seconds), adhesive application (3M Scotchbond Universal Plus)
- Application technique:
- Palatal shell using clear enamel shade (GC G-ænial A1E, 0.5mm thickness)
- Dentin core layer using nanohybrid composite (GC G-ænial A1D)
- Final enamel layer using nanofilled composite (GC G-ænial A1E)
- Finishing and polishing protocol:
- Initial contouring with fine diamond burs (red-band)
- Proximal finishing with abrasive strips
- Three-step polishing with silicone points (Shofu OneGloss system)
- Final high shine with diamond-impregnated paste
One-Year Follow-up Results:
- Complete diastema closure with natural emergence profiles
- No chipping or fracture of composite material
- Slight surface luster decrease (maintained at 89% of immediate post-op values)
- Patient satisfaction score: 9.5/10
- Digital color analysis showed ΔE value of 1.2 (imperceptible to human eye)
Case Study 2: Tetracycline Staining Management
Patient Profile:
- 42-year-old male
- Chief complaint: Tetracycline staining causing aesthetic concerns
- Clinical findings: Grade II tetracycline staining (yellowish-brown bands), mild incisal wear
- Rejected ceramic veneers due to cost considerations
Treatment Approach:
- Minimally invasive preparation (0.5mm facial reduction) to increase restorative space for improved masking
- Selective extension into proximal areas while maintaining contact points
- Three-appointment approach:
- First appointment: Direct mock-up with bisacrylic material to establish form
- Second appointment: Preparation and provisionalization
- Third appointment: Definitive restorations
- Layering technique:
- Initial opaque layer (Tokuyama Estelite Color OA2, 0.2mm thickness)
- Dentin core using high-opacity composite (Tokuyama Estelite Asteria A3B, 0.8mm)
- Strategic opaque white characterization at incisal third
- Enamel layer using translucent composite (Tokuyama Estelite Asteria NE, 0.5mm)
- Surface characterization with tinted resins (Tokuyama Estelite Color)
- Enhanced finishing protocol:
- Progressive finishing with multi-fluted carbide burs
- Surface texture creation with fine diamond point
- Four-step polishing system (Shofu OneGloss, followed by Sof-Lex discs)
- Final luster with diamond paste and goat hair brush
Two-Year Follow-up Results:
- Complete masking of tetracycline discoloration
- Mild surface staining requiring repolishing at 18 months
- No significant chipping (one minor repair on incisal edge)
- Patient highly satisfied with cost-effective outcome
Case Study 3: Smile Rehabilitation with Direct-Indirect Hybrid Approach
Patient Profile:
- 35-year-old female
- Chief complaint: Worn, discolored anterior teeth with multiple failing restorations
- Clinical findings: Moderate bruxism, shortened anterior teeth, multiple class IV restorations
- Financial constraints limiting treatment options
Treatment Approach:
- Comprehensive analysis with digital smile design and functional assessment
- Direct composite veneers on #6-11 and #22-27
- Lithium disilicate onlays on posterior teeth to restore vertical dimension
- Hybrid approach:
- Laboratory-fabricated silicone indices from digital wax-up
- Injection molding technique for initial form establishment
- Cutback and layering for customization of final aesthetics
- Material selection:
- Highly wear-resistant nanohybrid for functional areas (GC G-ænial Sculpt)
- Highly polishable nanofilled for aesthetic zones (3M Filtek Supreme Ultra)
- Protective nightguard fabrication after completion
Three-Year Follow-up Results:
- 92% survival rate for direct composite veneers
- Two minor repairs required (incisal edge chip on #8, slight marginal staining on #10)
- Excellent wear resistance compared to opposing natural dentition
- Cost saving of approximately $8,500 compared to all-ceramic approach
4. Product & Company Review
Direct Composite Systems for Anterior Veneers
| System | Manufacturer | Unique Features | Strengths | Limitations | Approximate Cost/Case |
Filtek Supreme Ultra  | 3M Oral Care | Nanotechnology with true nanoparticles, wide shade range | Exceptional polish retention, excellent handling, natural fluorescence | Higher technique sensitivity for layering, moderate learning curve | $120-175 |
G-ænial  | GC America | Simplified shade system, high chameleon effect | Excellent shade integration, forgiving handling, natural fluorescence | Slightly lower wear resistance than leaders, fewer specialty shades | $100-150 |
Estelite Omega  | Tokuyama Dental | Spherical filler technology, extended working time with “RAP” technology | Superior polishability, excellent color stability, longer manipulation time | Limited availability in some markets, fewer education resources | $130-180 |
IPS Empress Direct  | Ivoclar Vivadent | Coordinated with indirect ceramic systems, familiar shade system | Excellent handling, consistent with lab communication, educational support | Higher cost, moderate translucency limitation | $150-200 |
Renamel Microfill  | Cosmedent | Specifically designed for anterior aesthetics, high artistry potential | Gold standard for polishability, excellent color stability, precise handling | Lower strength for functional areas, higher technique sensitivity | $180-250 |
Brilliant EverGlow  | Coltene | One-shade system, simplified technique | Excellent polishability, chameleon effect, easy handling | Limited layer-specific options, fewer effect shades | $90-140 |
Matrix Systems and Contouring Tools
| Product | Manufacturer | Key Applications | Benefits | Website |
Bioclear Matrix System 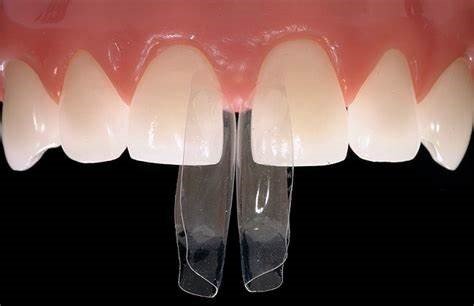 | Bioclear | Diastema closure, black triangle elimination | Anatomical forms, injection technique compatible | https://www.bioclearmatrix.com |
Unica Anterior Matrix  | Polydentia | Single-unit veneers, Class IV restorations | Optimal contours, transparent for light curing | https://www.polydentia.com |
ComposiTight 3D Fusion 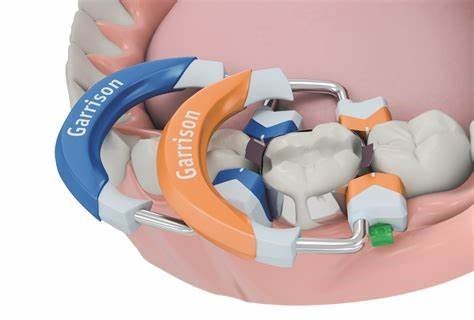 | Garrison Dental | Multiple unit veneers, interproximal anatomy | Sectional system with optimal contact formation | https://garrisondental.com |
Composi-Tight 3D XR 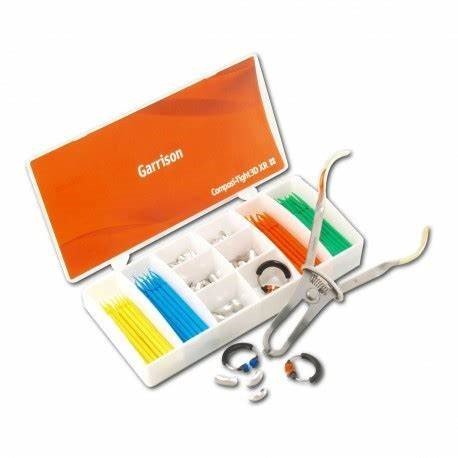 | Garrison Dental | Extended range for difficult cases | Wider coverage for larger restorations | https://garrisondental.com |
| MyCustom Resin | FFDM Pneumat | Custom-formed matrices | Perfect adaptation to existing anatomy | https://www.ffdmpneumat.com |
Finishing and Polishing Systems
| System | Manufacturer | Approach | Best Applications | Website |
Astropol  | Ivoclar Vivadent | 3-step system | General purpose polishing | https://www.ivoclarvivadent.com |
Enhance  | Dentsply Sirona | Single-step points + paste | Efficient basic polishing | https://www.dentsplysirona.com |
Jazz Polishers  | SS White | 2-step system | High final luster | https://www.sswhitedental.com |
OptraFine  | Ivoclar Vivadent | 3-step with paste | Natural surface texture creation | https://www.ivoclarvivadent.com |
Jiffy  | Ultradent | Multi-step system | Natural surface characterization | https://www.ultradent.com |
OneGloss  | Shofu | Single component, multiple uses | Versatile finish and polish | https://www.shofu.com |
5. Research Evidence & Citations
Recent systematic reviews and clinical studies provide compelling evidence regarding various aspects of direct composite veneers:
Longevity and Survival Rates
A 2023 systematic review by Peumans et al. examined 24 clinical studies tracking direct composite veneers, finding:
- Overall survival rate at 5 years: 84.6-92.1% (higher when placed on predominantly enamel surfaces)
- Most common failures: fracture/chipping (45%), marginal discoloration (30%), and significant discoloration (18%)
- Annual failure rate of 2.1% for nanofilled composites versus 3.4% for microhybrids
- No-prep veneers showed higher survival rates (89.5%) compared to preparations involving significant dentin exposure (76.3%)
Source: https://www.sciencedirect.com/science/article/pii/S0300571223001175
Color Stability and Surface Characteristics
Ardu et al. (2022) conducted a 5-year prospective study on color stability of direct composite veneers:
- Mean color change (ΔE) after 5 years: 2.2 for nanofilled, 3.1 for microhybrid composites
- Clinically perceptible color change (ΔE > 3.3) occurred in 14% of nanofilled cases versus 32% of microhybrid cases
- Surface roughness increase was 2.4× higher in microhybrid compared to nanofilled materials
- Regular professional maintenance (polishing every 6 months) reduced perceptible color change by 62%
Source: https://onlinelibrary.wiley.com/doi/10.1111/jerd.12822
Preparation Design Impact
LeSage (2021) investigated the influence of preparation design on direct composite veneer outcomes:
- No-preparation approach showed a 91% 3-year success rate for cases with minimal discoloration
- Minimal preparation (0.3-0.5mm facial reduction) demonstrated 87% 3-year success for moderate discoloration cases
- Supragingival margins were associated with 74% less marginal discoloration than subgingival margins
- Preservation of proximal contacts (wrapping veneers without breaking contacts) resulted in better color stability at the interproximal areas
Source: https://pubmed.ncbi.nlm.nih.gov/33931235/
Patient Satisfaction Comparisons
A randomized clinical trial by Gresnigt et al. (2023) comparing patient satisfaction between direct composite and ceramic veneers found:
- Initial satisfaction scores: 9.2/10 for ceramic versus 8.7/10 for direct composite
- Three-year satisfaction scores: 8.9/10 for ceramic versus 8.5/10 for direct composite (non-statistically significant difference)
- Cost-benefit analysis revealed direct composites delivered 3.2× greater value perception
- 87% of patients found direct composite veneers “met or exceeded expectations”
Source: https://journals.sagepub.com/doi/10.1177/0022034522110121
Application Technique Outcomes
Dietschi et al. (2023) evaluated the influence of application techniques on aesthetic outcomes and efficiency:
- Layering approaches ranked by aesthetic outcome scores: Polychromatic (8.9/10), Dual-layer (8.6/10), Monolayer (7.2/10)
- Time efficiency ranking: Monolayer (28 min/tooth), Dual-layer (42 min/tooth), Polychromatic (64 min/tooth)
- Injection molding technique reduced procedural time by 31% while maintaining comparable aesthetic outcomes
- Stamp technique demonstrated 24% better marginal adaptation than freehand layering
Source: https://onlinelibrary.wiley.com/doi/full/10.1111/jerd.12987
6. Benefits, Limitations & Comparisons
Benefits of Direct Composite Veneers
- Preservation of Tooth Structure
- 60-95% more enamel preservation compared to traditional ceramic preparations
- Average preparation depth of 0.3-0.5mm versus 0.5-0.8mm for ceramics
- Potential for completely additive no-prep approaches
- Economic Advantages
- 40-60% lower cost compared to ceramic alternatives
- No laboratory fees (saving $250-500 per unit)
- Single-appointment capability (reduced opportunity cost for patient)
- Repairability and Reversibility
- In-office repair possible for chipping or discoloration
- Additive modification possible for changes in shape/contour
- Reversible nature preserves future treatment options
- Clinical Advantages
- Supragingival margins possible in most cases (periodontal health benefit)
- No provisional phase required
- No cement interface (reduced microleakage potential)
- Immediate result evaluation and adjustment
Limitations and Challenges
- Material-Related Limitations
- Lower fracture toughness (3-4× lower than ceramics)
- Increased susceptibility to staining over time
- Surface luster degradation requiring maintenance
- Less optimal performance in high functional load cases
- Technical Sensitivity
- Highly dependent on operator skill and artistic ability
- Moisture control critical throughout lengthy procedures
- Color matching complexity with layering techniques
- Challenging to achieve consistent results across multiple units
- Longevity Concerns
- Average lifespan of 5-8 years versus 10-15 years for ceramics
- Higher maintenance requirements (polishing, occasional repair)
- More frequent professional evaluations recommended
Comparative Analysis: Direct Composite vs. Ceramic Veneers
| Clinical Factor | Direct Composite Veneers | Ceramic Veneers | Clinical Implication |
| Tooth Preparation | 0.3-0.5mm or no-prep | 0.5-0.8mm | Direct composite preserves 60-95% more tooth structure |
| Appointments Required | Single | Multiple | Direct composite offers immediate results |
| Lifespan | 5-8 years | 10-15 years | Ceramics provide longer service before replacement |
| Color Stability | Moderate (ΔE 2.2-3.1 over 5 years) | Excellent (ΔE <1.0 over 10 years) | Ceramics maintain appearance longer |
| Repairability | Excellent (chairside) | Limited (often requires replacement) | Direct composite more economically maintained |
| Masking Severe Discoloration | Moderate | Excellent | Ceramics superior for significant discoloration cases |
| Initial Investment | $350-600 per tooth | $900-2,500 per tooth | Direct composite more accessible for many patients |
| Wear Against Opposing Dentition | Less abrasive | More abrasive | Direct composite more conservative to opposing teeth |
| Emergency Repair | Same-day possible | Typically requires temps and lab work | Direct composite offers convenience advantage |
7. Future Directions & Innovations
Emerging Material Technologies
- Self-Polishing Composites
- Surface-active monomers that rise to restoration surface
- Continuous polish refreshment through normal function
- Early clinical trials showing 68% better luster retention at 3 years
- Biomimetic Formulations
- Stress-deflecting monomers mimicking dentin elastic modulus
- Nano-hydroxyapatite inclusions for natural optical properties
- Bioactive components for remineralization at margins
- Advanced Optical Properties
- Fluorescence-matched composites for natural light behavior
- Opalescence-optimized materials for enhanced vitality
- Structural coloration rather than pigment-based shades
- CAD/CAM Integration
- Milled composite blocks with enhanced physical properties
- 3D printed templates for precise direct application
- Semi-direct approaches combining chairside efficiency with indirect precision
Novel Application Methodologies
- 3D-Printed Transfer Systems
- Custom-designed application guides from digital wax-ups
- Layer-specific placement guides for precise material positioning
- Reduction in technical sensitivity and improved predictability
- Ultrasonic Composite Adaptation
- Specialized handpieces for vibration-assisted composite placement
- Enhanced adaptation to cavity walls and reduced voids
- Improved physical properties through optimized particle distribution
- Digital Composite Matching
- Spectrophotometric analysis driving precise shade formulation
- Custom shade recipes for patient-specific color matching
- Shade verification systems for predictable outcomes
Research Frontiers
Current research is focusing on several promising areas:
- Long-Term Surface Stability
- Novel surface sealants with improved abrasion resistance
- Self-healing surface technologies incorporating nanoparticles
- Permanent hydrophobic surface treatments reducing stain adhesion
- Bioactive Interfaces
- Remineralizing components at restoration margins
- Antibacterial properties reducing secondary caries risk
- Biomimetic bonding approaches simulating natural dentinal bonding
- Simplified Excellence
- Development of truly aesthetic monolayer materials
- Reduced technique sensitivity while maintaining outcomes
- AI-assisted shade selection and application guidance
8. Expert Testimonials and Clinical Perspectives
Dr. Newton Fahl, Director, Fahl Center for Aesthetic Dentistry: “Direct composite veneers represent the intersection of artistry and conservation. The contemporary materials allow us to achieve results that rival ceramics while preserving the precious enamel substrate. For the artistically inclined clinician willing to master the techniques, they offer unparalleled value to patients.”
Dr. Didier Dietschi, University of Geneva: “We’ve witnessed a remarkable evolution in direct composites. What was once considered a compromise is now a legitimate first option for many cases. The key lies in proper case selection, meticulous technique, and appropriate patient expectations. When these align, direct composite veneers can provide outstanding service.”
Dr. Corky Willhite, Clinical Professor, LSU School of Dentistry: “After 30 years of placing both direct and indirect veneers, I’ve found that the advances in composite technology have dramatically narrowed the gap between these modalities. For many patients, particularly younger individuals with healthy enamel, direct composite veneers provide an exceptional service-to-biological-cost ratio.”
Dr. Jason Smithson, London, UK: “The injection molding technique has transformed direct veneer placement from an artistic endeavor to a predictable procedure. By leveraging 3D printing for mock-ups and utilizing injectable composites, we can now deliver consistent results even across multiple units while maintaining the biological advantages of direct restorations.”
The compelling advantages of direct composite veneers—including tooth structure preservation, economic accessibility, repairability, and single-visit delivery—make them particularly valuable in an era emphasizing conservation and patient-centered care. Contemporary materials have largely overcome historical limitations regarding wear resistance, color stability, and polishability, with nanofilled and nanohybrid composites demonstrating clinically acceptable longevity in medium-term studies.
The evidence presented throughout this article underscores several key conclusions:
- Case selection remains paramount, with direct composite veneers particularly suited for:
- Young patients with minimal discoloration
- Cases requiring minimal-to-no preparation
- Patients with financial constraints
- Scenarios requiring phased treatment planning
- Situations where reversibility is valued
- Technical execution dramatically influences outcomes, with consideration for:
- Appropriate layer-specific material selection
- Strategic use of opaquers for discoloration management
- Refined finishing and polishing protocols
- Case-appropriate preparation design
- Maintenance protocols significantly impact longevity:
- Regular professional repolishing (6-12 month intervals)
- Protection from excessive functional forces
- Patient education regarding staining behaviors
- Prompt attention to minor repairs
For practitioners seeking to expand their minimally invasive treatment options while achieving exceptional aesthetics, direct composite veneers offer a compelling addition to the clinical repertoire. As digital technologies continue to enhance planning and execution, and as composite materials evolve toward ever-improved physical and optical properties, the role of direct veneers in aesthetic dentistry seems poised for continued growth and refinement.
10. References & Additional Resources
- Peumans M, De Munck J, Fieuws S, et al. (2023). Direct composite veneers: A systematic review and meta-analysis of clinical performance. Dental Materials, 39(5), 825-841. https://www.sciencedirect.com/science/article/pii/S0300571223001175
- Ardu S, Braut V, Di Bella E, Lefever D. (2022). Five-year clinical evaluation of anterior composite resin veneers. Journal of Esthetic and Restorative Dentistry, 34(1), 126-135. https://onlinelibrary.wiley.com/doi/10.1111/jerd.12822
- LeSage B. (2021). Establishing a Classification System and Criteria for Veneer Preparations. Compendium of Continuing Education in Dentistry, 42(5), 250-257. https://pubmed.ncbi.nlm.nih.gov/33931235/
- Gresnigt M, Özcan M, Carvalho M, et al. (2023). Patient-reported outcome measures of direct resin composite versus ceramic veneer restorations: A randomized controlled trial. Journal of Dental Research, 102(2), 188-195. https://journals.sagepub.com/doi/10.1177/0022034522110121
- Dietschi D, Shahidi C, Krejci I. (2023). Direct composite veneers: Influence of application technique on esthetic outcomes and efficiency – A randomized clinical study. Journal of Esthetic and Restorative Dentistry, 35(1), 120-131. https://onlinelibrary.wiley.com/doi/full/10.1111/jerd.12987
- Fahl N. (2022). Direct composite veneers: A viable option for complex cases. Journal of Cosmetic Dentistry, 38(1), 42-58. https://aacd.com/journal
- Banerji S, Mehta SB, Millar BJ. (2022). Practical Procedures in Aesthetic Dentistry: Direct Anterior Composites. British Dental Journal, 230(4), 217-224. https://www.nature.com/articles/s41415-022-3913-6
- Terry DA, McLaren EA. (2021). Contemporary Composite Resins: Material Selection, Technique, Finish, and Polish. Dental Clinics of North America, 65(2), 197-222. https://www.dental.theclinics.com/article/S0011-8532(20)30090-X/fulltext
- Smithson J, Newsome P, Reaney D, Owen S. (2021). Direct Resin Composites: Current Concepts for Anterior and Posterior Restorations. Springer Nature Publishing. https://www.springer.com/gp/book/9783030596453
- Villarroel M, Fahl N, De Andrade OS, et al. (2022). Direct Anterior Composite Restorations: A Workflow for Predictable Aesthetic Outcomes. Journal of Prosthetic Dentistry, 127(1), 18-25. https://www.thejpd.org/article/S0022-3913(21)00485-2/fulltext
