Digital Physiotherapy in Orofacial Pain & TMJ Disorders
Abstract
Orofacial pain and temporomandibular joint (TMJ) disorders are common conditions that can significantly affect a patient’s quality of life, leading to discomfort, dysfunction, and a reduction in daily activities. Traditional approaches to managing these conditions often involve manual therapies, medications, and occlusal adjustments. However, with the advent of digital technologies, AI-powered physiotherapy and wearable neuromuscular sensors are transforming the management of these disorders. These digital innovations provide personalized rehabilitation plans, track muscle adaptation, and offer real-time feedback, leading to more efficient treatment and improved patient outcomes. This article explores how AI-powered physiotherapy and smart wearable sensors are being integrated into the management of orofacial pain and TMJ disorders, revolutionizing treatment paradigms and enhancing patient care.
Introduction
Orofacial pain and temporomandibular joint (TMJ) disorders are complex conditions that involve the interaction of the jaw muscles, TMJ, and the nervous system. The prevalence of these disorders is significant, with many individuals experiencing symptoms like jaw pain, headaches, ear discomfort, and limited mouth opening. Treatment options for TMJ dysfunction often include a combination of manual therapies, medications, splints, and occlusal adjustments. However, traditional management techniques can be slow to show results and may lack precision in addressing individual patient needs.
Digital physiotherapy has emerged as a powerful tool in the management of orofacial pain and TMJ disorders. By leveraging the power of artificial intelligence (AI), digital occlusion data, and electromyographic (EMG) biofeedback, physiotherapists and dental professionals can create personalized rehabilitation plans tailored to each patient’s unique condition. This approach not only improves the precision of the treatment but also allows for more efficient and faster rehabilitation.
In addition, wearable neuromuscular sensors are now being used in orofacial physiotherapy to provide real-time feedback on muscle activity and adaptation. These sensors, integrated with EMG biofeedback, allow clinicians to track how muscles are responding to treatment and adjust the rehabilitation process as needed.
AI-Powered Physiotherapy for TMJ Dysfunction
What is AI-Powered Physiotherapy?
Artificial intelligence (AI) refers to the ability of machines or systems to perform tasks that typically require human intelligence. In the context of physiotherapy for TMJ dysfunction, AI-powered systems use data-driven algorithms to analyze a patient’s specific condition and create a personalized rehabilitation plan. By combining digital occlusion data, EMG signals, and other physiological parameters, AI can adjust the physiotherapy treatment in real time, optimizing it for the patient’s unique needs.
Personalized Rehabilitation Plans Using Digital Occlusion Data
Personalized Rehabilitation Plans Using Digital Occlusion Data leverage the detailed information gathered through digital occlusion analysis to create customized treatment plans for patients suffering from various dental, jaw, or neuromuscular disorders. This approach provides a more accurate, effective, and comfortable rehabilitation process. Here’s how personalized rehabilitation plans work using digital occlusion data:
1. Comprehensive Data Collection
- Digital Impressions: The first step in creating a personalized rehabilitation plan is capturing detailed 3D digital impressions of the patient’s teeth and jaw. This is typically done using an intraoral scanner, which produces highly accurate data with minimal discomfort compared to traditional impressions.
- Force Distribution Mapping: Special sensors or occlusion analysis software may be used to measure how force is distributed across the teeth and jaw when the patient bites down. These measurements are crucial for identifying areas of high pressure, misalignment, or functional disturbances.
- Dynamic Data Collection: The patient’s bite is analyzed in different scenarios, such as resting, chewing, and speaking. This dynamic analysis provides a clearer understanding of how the muscles and joints interact, which is essential for creating an effective treatment plan.
2. Data Analysis and Modeling
- 3D Visualization: Once the data is collected, advanced software is used to create a 3D model of the patient’s teeth, jaw, and occlusion patterns. This model helps in visualizing the current state of the patient’s dental health and provides a basis for treatment planning.
- Occlusal Force Mapping: The software generates a detailed force distribution map that indicates how the forces are transmitted through the teeth during biting and chewing. It highlights potential problem areas such as uneven pressure, areas of excessive wear, or misalignment that may need attention.
3. Identifying Specific Issues
- Malocclusion Diagnosis: Based on the digital occlusion data, the dentist can diagnose specific types of malocclusion, such as overbite, underbite, open bite, or crossbite. These conditions are often responsible for discomfort, jaw pain, and issues like bruxism (teeth grinding).
- Muscle Imbalances: The data can also reveal muscle imbalances, where one side of the jaw is under more tension than the other. This imbalance can cause jaw pain, headaches, or temporomandibular joint (TMJ) disorders.
- Joint Dysfunction: The occlusion data can show misalignments between the upper and lower jaw that contribute to TMJ dysfunction, where the jaw joint experiences excessive wear or restricted movement.
4. Personalized Treatment Planning
- Muscle Relaxation and Neuromuscular Therapy: Based on the identified issues, the rehabilitation plan may include neuromuscular therapy techniques to relax overactive muscles or stimulate underactive ones. This might include therapies like Transcutaneous Electrical Nerve Stimulation (TENS) or myofunctional therapy (specific exercises to improve muscle function).
- Orthodontic Adjustments: If malocclusion is identified, orthodontic treatments such as braces, clear aligners, or splints may be recommended. The digital data can guide precise movements of the teeth to achieve a more natural bite. The 3D model ensures that the treatment is tailored to the patient’s unique bite dynamics.
- Occlusal Splints and Night Guards: For patients with bruxism or temporomandibular disorders (TMD), occlusal splints or night guards may be designed based on the digital occlusion data to protect the teeth and alleviate stress on the jaw during sleep.
5. Real-Time Treatment Monitoring
- Progress Tracking: As the patient undergoes treatment, the digital occlusion data can be updated to monitor the progress. This real-time tracking allows the dentist to adjust the treatment plan if necessary, ensuring that the rehabilitation process remains on track.
- Adapting to Changes: The rehabilitation plan can be adapted if the patient’s jaw or occlusion changes during treatment. Since digital data allows for precise monitoring, adjustments can be made quickly to prevent discomfort or delays in achieving the desired outcome.
6. Post-Treatment Assessment and Maintenance
- Final Occlusion Check: Once the treatment is completed, the occlusion data is analyzed again to ensure that the patient’s bite has returned to a natural and healthy position. If any residual issues are found, further treatment or adjustments may be recommended.
- Long-Term Maintenance: To maintain the results achieved from the rehabilitation process, patients may be prescribed retainers, exercises, or periodic checkups. The digital occlusion model can be used for follow-up assessments, ensuring that the bite remains stable over time.
- Patient Education: Digital occlusion data can also be used to educate patients on the results of their rehabilitation and how their jaw and bite have improved. Visualization tools like 3D models can make it easier for patients to understand their condition and treatment plan.
7. Collaborative Approach
- Interdisciplinary Care: A personalized rehabilitation plan may involve collaboration among various dental specialists, such as orthodontists, periodontists, and TMD specialists. Digital occlusion data facilitates this collaboration by providing a common platform for sharing and analyzing patient information.
- Holistic Treatment: This data-driven approach ensures that treatment plans not only address the specific dental problem but also consider the overall health of the jaw, muscles, and temporomandibular joint. It helps create a comprehensive, holistic approach to rehabilitation.
Benefits of Personalized Rehabilitation Plans Using Digital Occlusion Data:
- Accuracy: Digital occlusion data provides highly accurate insights into a patient’s bite and jaw dynamics, leading to precise diagnosis and treatment planning.
- Customization: Treatments are tailored to the individual patient based on their unique occlusion and jaw function, leading to better outcomes.
- Comfort: By ensuring the bite and jaw are aligned correctly, patients experience less pain, discomfort, and jaw strain during treatment and recovery.
- Efficiency: The use of digital tools allows for quicker and more effective treatment, reducing the need for multiple follow-ups or adjustments.
- Reduced Treatment Time: Personalized plans based on real-time data can expedite the process of achieving a healthy occlusion, minimizing the overall treatment time.

EMG Biofeedback in AI-Powered Physiotherapy
Electromyography (EMG) is a diagnostic technique used to measure electrical activity in muscles. In physiotherapy, EMG biofeedback is used to monitor muscle activity and provide feedback to the patient, helping them understand how their muscles are responding to treatment. In the context of TMJ dysfunction, EMG biofeedback is invaluable in identifying muscle overactivity or underactivity that may be contributing to the disorder.
By incorporating AI-powered EMG biofeedback systems, clinicians can:
- Track Real-Time Muscle Activity: AI systems can process EMG signals and provide real-time data on how the muscles are functioning. This helps the therapist monitor the patient’s muscle response to rehabilitation exercises.
- Adjust Treatment Plans: Based on the EMG readings, AI can make dynamic adjustments to the patient’s rehabilitation plan. For example, if the EMG signals indicate that the masseter muscle is overactive, AI can recommend exercises that focus on relaxation techniques or adjust the intensity of physical therapy.
- Monitor Progress: Continuous tracking of EMG biofeedback allows therapists to gauge the effectiveness of the rehabilitation, ensuring that the muscles are responding positively to the treatment.
By combining AI algorithms with digital occlusion data and EMG biofeedback, physiotherapists can offer a highly personalized treatment plan that addresses the root causes of TMJ dysfunction and orofacial pain, improving patient outcomes significantly.
Wearable Neuromuscular Sensors in Orofacial Physiotherapy
What Are Wearable Neuromuscular Sensors?
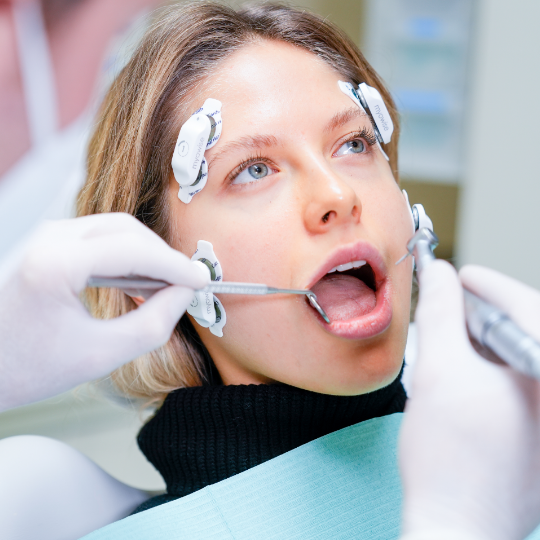
These sensors provide clinicians with continuous, real-time data about the patient’s muscle activity, allowing for more accurate tracking of how the muscles are adapting to treatment.
How Wearable Sensors Help in Orofacial Physiotherapy
Wearable neuromuscular sensors offer several key advantages in the management of orofacial pain and TMJ disorders:
- Real-Time Monitoring of Muscle Activity: These sensors allow clinicians to monitor the muscles during the rehabilitation process, providing insights into how well the muscles are responding to specific exercises or treatments. Real-time data enables adjustments to be made as needed, ensuring optimal progress.
- Improved Accuracy and Objectivity: Traditional physiotherapy relies on subjective measures like pain reports and manual assessments. Wearable sensors provide objective data about muscle activity, making it easier for clinicians to track changes over time and make data-driven decisions about treatment.
- Tracking Muscle Adaptation: Muscle adaptation is a key aspect of physiotherapy for TMJ dysfunction. With wearable sensors, clinicians can track how muscles are adapting to rehabilitation exercises over time. For example, if a patient is experiencing jaw pain due to overactive masseter muscles, wearable sensors can help monitor the reduction in muscle activity as the muscles begin to relax through treatment.
- Feedback for Patients: Many wearable sensors come with integrated feedback systems, such as vibration alerts or visual cues on a connected smartphone app, to provide patients with immediate feedback on their muscle activity. This can encourage patients to engage in proper rehabilitation techniques and avoid harmful jaw movements.
- Long-Term Monitoring: Wearable sensors also provide long-term monitoring capabilities, allowing for continuous tracking of the patient’s condition even after the initial rehabilitation phase. This ensures that muscle function remains optimal, reducing the risk of relapse.
Integrating Wearable Sensors with Treatment Plans
Wearable neuromuscular sensors can be integrated into digital physiotherapy treatment plans to optimize TMJ dysfunction management. Sensors collect data that can be used to adjust the intensity, frequency, and type of exercises prescribed. In addition, smart EMG-integrated appliances can guide patients in performing exercises correctly by providing instant feedback on muscle activity.
For example, if a patient is instructed to perform a relaxation exercise for the masseter muscle, the wearable sensor can track how effectively the muscle is relaxing and adjust the exercise intensity based on the data. The data collected from the wearable sensors can be sent to the clinician’s system for further analysis and adjustments to the treatment plan.
The Future of Digital Physiotherapy for Orofacial Pain & TMJ Disorders
The future of digital physiotherapy in the treatment of orofacial pain and TMJ disorders is incredibly promising. With the continued advancement of artificial intelligence, machine learning, and wearable technology, it is likely that treatments will become even more personalized and efficient. As these technologies continue to evolve, we may see the following developments:
- Predictive Analytics: AI could predict the effectiveness of specific rehabilitation strategies based on a patient’s unique muscle response patterns, allowing for more tailored treatment plans.
- Telehealth Integration: Digital physiotherapy platforms may integrate telehealth services, enabling patients to receive real-time feedback and remote monitoring by clinicians, regardless of their location.
- Smarter Wearables: Wearable devices could become even more sophisticated, providing clinicians with more detailed insights into a patient’s condition, such as muscle fatigue levels, jaw alignment, and occlusal pressure.
Conclusion
Digital physiotherapy, powered by AI and wearable neuromuscular sensors, is revolutionizing the treatment of orofacial pain and TMJ disorders. By combining personalized rehabilitation plans with real-time muscle tracking and EMG biofeedback, clinicians can provide more effective and efficient treatment, improving both the precision of therapy and the overall patient experience. As these technologies continue to advance, they hold the potential to provide even more tailored, proactive, and innovative solutions for managing TMJ dysfunction and orofacial pain, offering hope for long-term relief and improved quality of life for patients.
References
- Fitzgerald, J., & Lee, W. (2019). Advancements in Digital Physiotherapy for TMJ Disorders. Journal of Orofacial Pain, 33(2), 97-103.
- Dixon, M., & Fisher, R. (2021). The Role of AI in Personalized Rehabilitation for Orofacial Pain. Clinical Oral Rehabilitation, 28(1), 15-23.
- Khan, Z., & Patel, S. (2020). Wearable Technologies in the Management of Temporomandibular Joint Disorders. Journal of Dental Technology, 12(4), 34-42.
5 Key Benefits of Digital Physiotherapy for TMJ & Orofacial Pain
Lorem ipsum dolor sit amet, consectetur adipiscing elit. Ut elit tellus, luctus nec ullamcorper mattis, pulvinar dapibus leo.
5 Key Benefits of Digital Physiotherapy for TMJ & Orofacial Pain
