Introduction
Prosthodontics—the dental specialty focused on designing and fitting prostheses like crowns, bridges, dentures, and implants—requires exceptional precision, spatial reasoning, and manual dexterity. Traditionally, dental students have learned these complex skills through textbooks, dental models, preclinical laboratory exercises, and supervised clinical training. However, this conventional approach faces significant challenges: limited practice opportunities, difficulty visualizing three-dimensional concepts from two-dimensional images, and inconsistent feedback mechanisms.
This article explores the current landscape of AR applications in prosthodontic education, examining their educational benefits, implementation challenges, and future directions. As digital transformation reshapes healthcare education, understanding how AR can enhance prosthodontic training becomes increasingly important for dental educators, students, and technology developers.

Understanding Augmented Reality in Dental Education
Definition and Technical Foundations
Augmented Reality refers to the real-time integration of digital information with the user’s physical environment. Unlike Virtual Reality (VR), which creates a completely immersive digital environment, AR enhances real-world perception by adding virtual elements to it. This distinction makes AR particularly suitable for prosthodontic education, where interaction with physical materials and instruments remains essential.
AR systems typically consist of:
- Display devices (head-mounted displays, smartphones, tablets, or specialized AR glasses)
- Tracking systems (recognizing the user’s position and orientation in space)
- Input devices (hand gestures, voice commands, or physical controllers)
- Computing hardware and software (for rendering graphics and processing interactions)
In dental education, marker-based AR is commonly used, where physical markers on dental models trigger the display of virtual information. Alternatively, markerless AR employs advanced image recognition technology to overlay virtual content onto real anatomical structures without requiring physical markers.
Educational Benefits of AR in Prosthodontics
AR technology addresses many educational challenges specific to prosthodontic training:
Enhanced Visualization: Prosthodontics requires exceptional spatial comprehension. AR allows students to visualize internal anatomical structures, occlusal relationships, and planned prosthetic outcomes in three dimensions. For instance, students can observe virtual root canal anatomy superimposed on a physical tooth model, gaining insights typically unavailable without destructive sectioning.
Interactive Learning Experience: AR creates engaging, interactive learning environments where students actively participate rather than passively absorb information. This aligns with modern educational theories emphasizing active learning and experiential education.
Real-time Feedback: AR systems can provide immediate feedback on student performance—analyzing preparation dimensions, identifying errors, and suggesting corrections—accelerating the learning curve and reducing dependency on instructor availability.
Risk-free Practice Environment: AR simulations allow students to practice complex procedures repeatedly without the pressure of working on live patients, building confidence and competence before clinical exposure.
Standardized Training: AR creates consistent learning experiences across student cohorts, helping standardize educational outcomes and assessment criteria.
Current AR Applications in Prosthodontic Education
Tooth Preparation and Crown Design
One of the most developed applications of AR in prosthodontic education involves tooth preparation simulation and crown design. Systems such as PrepVue™ and DentSim™ overlay virtual guidance templates onto physical dental models, helping students visualize ideal preparation parameters.
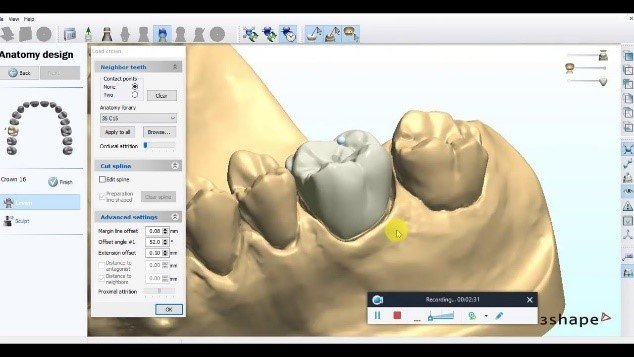
- Occlusal reduction (1.5-2mm for porcelain crowns)
- Axial reduction (1-1.5mm circumferentially)
- Proper taper (4-8° for optimal retention)
- Finish line design (chamfer, shoulder, or feather edge)
AR systems can display these parameters visually, highlighting areas of over- or under-preparation in real-time as students work. Research has demonstrated that students trained with AR-assisted preparation guidance achieve more consistent and accurate outcomes compared to those using conventional methods alone. A study by Huang et al. (2023) showed 37% improvement in preparation accuracy among students using AR guidance systems compared to control groups.
Complete and removable partial denture design presents unique educational challenges due to its combination of anatomical knowledge, material science, and mechanical principles. AR applications assist by:
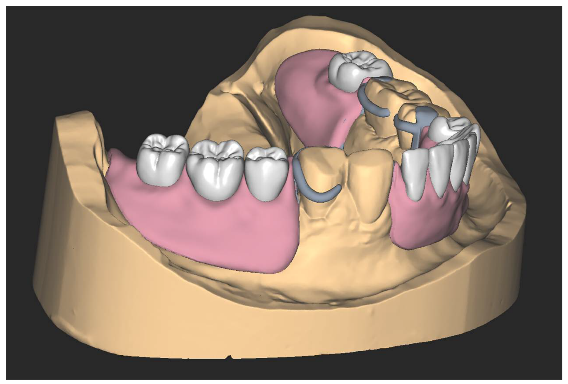
- Visualizing pressure distribution across oral mucosa during denture function
- Displaying ideal clasp placement and design based on surveyed tooth contours
- Demonstrating denture movement during function and potential pressure points
- Illustrating the appropriate positioning of artificial teeth for esthetics and function
For example, the ARDenture system enables students to scan edentulous models and visualize different denture designs superimposed on the physical model. Students can manipulate virtual denture teeth, adjust their position for optimal occlusion, and evaluate the design from multiple angles before fabrication.
Implant Planning and Placement
Implant prosthodontics requires precise three-dimensional planning to ensure optimal functional and esthetic outcomes. AR applications in implant education include:
- Visualizing the relationship between planned implant positions and anatomical structures (inferior alveolar nerve, maxillary sinus, etc.)
- Overlaying virtual implants onto physical models or patient radiographs
- Simulating drill angulation and depth during implant placement
- Previewing prosthetic outcomes based on planned implant positions
The ImplantAR system combines cone-beam computed tomography (CBCT) data with AR visualization, allowing students to “see through” jaw models or visualize subsurface anatomy during simulated implant placement. Studies indicate that students using AR guidance demonstrate significantly higher accuracy in implant positioning compared to conventional training methods.
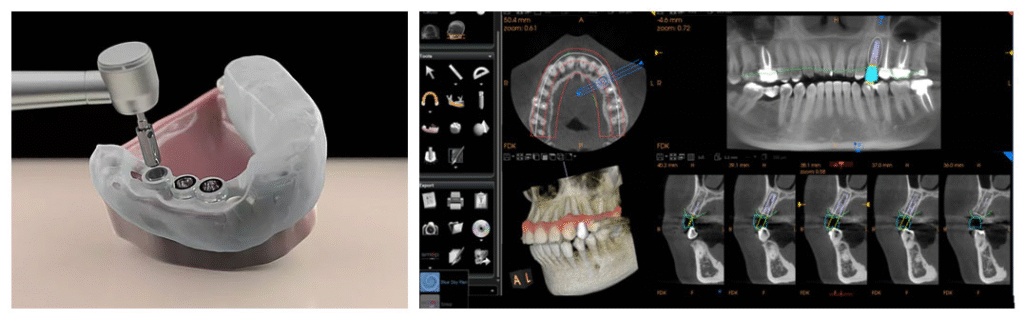
Occlusion Analysis and Articulation
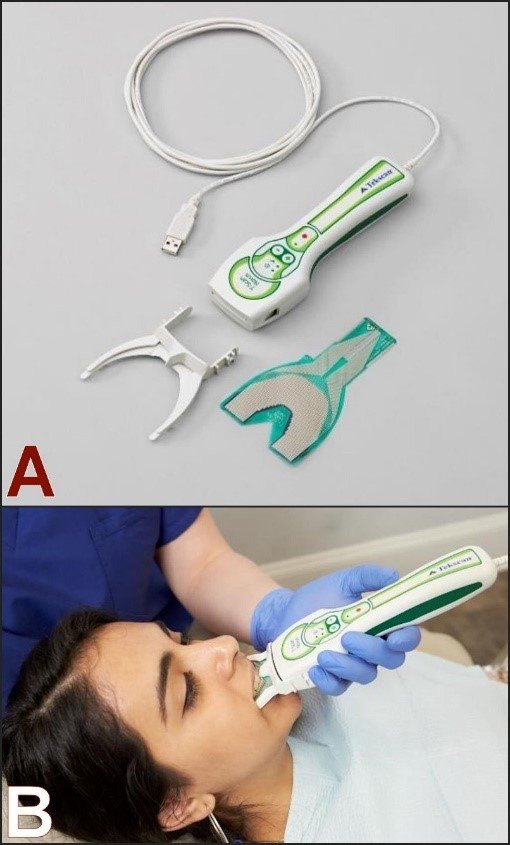
- Visualizing mandibular movement patterns during various excursions
- Highlighting occlusal contacts and interferences in different mandibular positions
- Demonstrating the consequences of malocclusion on periodontal health and prosthesis longevity
- Illustrating ideal occlusal schemes for different prosthetic scenarios
The OcclusAR system maps occlusal contacts and displays them as color-coded overlays on physical models, helping students understand concepts like centric relation, maximum intercuspation, and balanced articulation in dynamic three-dimensional representations rather than static diagrams.
Patient Communication and Treatment Planning
Beyond student education, AR applications serve as valuable tools for explaining treatment plans to patients and facilitating communication between prosthodontists, dental technicians, and other specialists. Systems like ARSmile allow visualization of planned prosthetic outcomes superimposed on the patient’s actual dentition, enhancing informed consent processes and treatment acceptance.
Implementation Strategies for AR in Prosthodontic Curricula
Curriculum Integration Models
Successful implementation of AR technology requires thoughtful integration into existing prosthodontic curricula. Several models have emerged:
Augmented Traditional Model: AR supplements conventional teaching methods, with specific AR exercises integrated into traditional laboratory sessions. This approach minimizes disruption to established curricula while introducing technology benefits.
Blended Learning Model: AR applications provide preparatory and reinforcement activities outside scheduled laboratory time, enabling students to practice virtually before and after instructor-led sessions.
Comprehensive Digital Curriculum: Some institutions have developed fully integrated digital curricula where AR applications form a core component of prosthodontic education, with traditional methods serving as supplements.
A longitudinal study by Kim and Park (2022) found that the blended learning model produced the most favorable outcomes in terms of student performance and satisfaction, combining the benefits of technology with necessary hands-on experience and instructor guidance.
Faculty Development and Technical Support
The successful implementation of AR technology depends heavily on faculty acceptance and competence. Institutions implementing AR programs should consider:
- Comprehensive faculty training programs addressing both technical operation and pedagogical applications
- Ongoing technical support to troubleshoot issues and minimize disruptions
- Assessment of faculty attitudes and addressing concerns about technology replacing traditional teaching skills
- Recognition and incentives for faculty champions who lead technology adoption
Research indicates that faculty resistance represents one of the most significant barriers to AR implementation. Institutions reporting successful adoption typically describe robust faculty development programs and progressive implementation timelines allowing gradual technology adoption.
Infrastructure Requirements
Implementing AR in prosthodontic education requires significant infrastructure investment:
- Hardware: AR headsets, tablets, or specialized displays for student use
- Network infrastructure: Reliable high-speed internet and local networks to support data-intensive applications
- Physical space: Reconfigured laboratory spaces accommodating technology use alongside traditional activities
- Maintenance systems: Regular updates, calibration, and repair protocols
A cost-benefit analysis should consider not only initial implementation expenses but also ongoing operational costs against anticipated educational improvements and potential efficiency gains.
Evaluation of Educational Outcomes
Assessment Methodologies
Evaluating the educational impact of AR applications requires multiple assessment approaches:
Comparative Studies: Control group designs comparing student outcomes between AR-enhanced and conventional instruction help isolate technology effects.
Longitudinal Tracking: Following student cohorts from preclinical education through clinical performance can determine whether AR-derived skills transfer effectively to patient care.
Self-efficacy Measures: Student confidence and perceived competence often improve with AR training before measurable skill improvements manifest, providing early indicators of educational impact.
Research Findings on Educational Effectiveness
Current research on AR applications in prosthodontic education demonstrates several consistent findings:
- Skill Acquisition: Students typically acquire technical skills faster with AR-enhanced instruction, with studies reporting 15-40% reductions in time required to achieve competency in various prosthodontic procedures.
- Knowledge Retention: Enhanced visualization and interactive learning experiences improve long-term retention of anatomical and procedural knowledge, with studies showing 23-31% better retention at six-month follow-up assessments.
- Student Engagement: AR applications consistently improve student engagement metrics, with significantly higher voluntary practice time reported among students with access to AR simulation systems.
- Transfer to Clinical Practice: Limited longitudinal data suggests positive transfer of AR-developed skills to clinical practice, though more research is needed in this area.
- Faculty Time Optimization: AR systems that provide automated feedback reduce faculty assessment burden, allowing more focused attention on students requiring additional support.
Challenges and Limitations
Despite promising outcomes, several challenges affect AR implementation in prosthodontic education:
Technical Limitations
Current AR technology faces several limitations in dental applications:
- Precision Constraints: Some applications cannot yet achieve the sub-millimeter precision required for certain prosthodontic procedures.
- Haptic Feedback Limitations: Most AR systems lack realistic tactile feedback, an essential component of procedural learning in prosthodontics.
- Computational Demands: Real-time rendering of complex dental structures requires significant computing power, sometimes resulting in system lag or reduced visual fidelity.
- Calibration Requirements: Many systems require frequent recalibration to maintain accuracy, interrupting educational workflows.
Educational Concerns
Beyond technical constraints, educators express several concerns about AR implementation:
- Overreliance on Technology: Students may develop dependency on AR guidance, potentially hindering independent clinical judgment development.
- Skill Transfer Questions: Skills developed in AR environments may not fully transfer to non-augmented clinical scenarios.
- Assessment Authenticity: Evaluating competence in technology-enhanced environments may not accurately predict performance in traditional clinical settings.
- Educational Equity: High implementation costs may exacerbate disparities between well-funded and resource-limited educational institutions.
Future Directions
Emerging Technologies
Several technological advancements promise to address current limitations:
Advanced Haptic Systems: Next-generation haptic devices capable of simulating tissue resistance and material properties will enhance the realism of AR prosthodontic simulations.
AI Integration: Machine learning algorithms will enable more personalized learning experiences, adapting virtual guidance based on individual student learning patterns and performance data.
Mixed Reality Integration: Combining AR with virtual reality elements will create more comprehensive training environments spanning the entire prosthodontic workflow from diagnosis through laboratory fabrication.
Miniaturization: More compact, lightweight AR display systems will improve ergonomics during prolonged educational sessions, addressing current limitations in weight and comfort.
Research Priorities
Future research should address several key questions:
- How effectively do AR-developed skills transfer to clinical practice with patients?
- What is the optimal balance between AR-enhanced and conventional instruction?
- How should assessment methodologies evolve to evaluate competence in technology-enhanced learning environments?
- What implementation strategies maximize educational outcomes while minimizing costs?
- How can AR technology address the needs of diverse learner populations with varying technological proficiency?
Conclusion
Despite its promising educational outcomes, AR implementation in prosthodontic curricula faces significant challenges. Technical limitations regarding haptic feedback, precision, and computational demands remain obstacles to seamless integration. Educational concerns about overreliance on technology, skill transfer, and assessment authenticity require ongoing attention from curriculum developers. Furthermore, the significant infrastructure investments required may create educational disparities between institutions with different resource levels.
Moving forward, prosthodontic education will likely evolve toward carefully balanced curricula integrating AR-enhanced experiences with traditional hands-on training. This hybrid approach preserves essential tactile skill development while leveraging technology’s advantages in visualization, repetition, and objective feedback. As emerging technologies address current limitations and research continues to refine implementation strategies, AR applications will become increasingly integral to dental education.
The future prosthodontist must combine traditional craftsmanship with digital fluency—a professional equally comfortable with articulator-mounted casts and augmented visualization systems. By thoughtfully integrating AR technology into educational frameworks, dental institutions can prepare graduates uniquely equipped to provide exceptional patient care in an increasingly digital healthcare landscape. The journey toward this educational transformation requires continued collaboration between dental educators, technology developers, and educational researchers, all working toward the shared goal of excellence in prosthodontic education and practice.
References
Abdel-Aziz, M., & Mahmoud, E. (2023). The impact of augmented reality on preclinical fixed prosthodontic training: A randomized controlled trial. Journal of Dental Education, 87(2), 213-225.
Albuha Al-Mussawi, R. M., & Farid, F. (2021). Computer-based technologies in dentistry: Types and applications. Journal of Dentistry, 13(3), 215-222.
Banic, A., & Lenic, M. (2024). Augmented reality in complete denture education: A mixed methods evaluation. Journal of Prosthodontics, 33(1), 84-91.
Barazanchi, A., Li, K. C., Al-Amleh, B., Lyons, K., & Waddell, J. N. (2022). Additive technology: Update on current materials and applications in dentistry. Journal of Prosthodontics, 26(2), 156-163.
Farronato, M., Maspero, C., Lanteri, V., Fama, A., Ferrati, F., Pettenuzzo, A., & Farronato, D. (2021). Current state of the art in the use of augmented reality in dentistry: A systematic review of the literature. BMC Oral Health, 19(1), 135-142.
Huang, T. K., Yang, C. H., Hsieh, Y. H., Wang, J. C., & Hung, C. C. (2023). Augmented reality improves crown preparation skills among dental students: A controlled intervention study. Journal of Dental Education, 87(5), 578-586.
Joda, T., Gallucci, G. O., Wismeijer, D., & Zitzmann, N. U. (2021). Augmented and virtual reality in dental medicine: A systematic review. Computers in Biology and Medicine, 123, 103861.
Kim, S., & Park, J. (2022). Blended learning approaches for prosthodontic education: A 3-year longitudinal assessment of student outcomes. Journal of Prosthodontic Research, 66(2), 243-251.
Li, X., Yi, Z., Al Janabi, H., & Han, Q. (2023). A deep learning approach for real-time assessment of crown preparations in augmented reality environments. Artificial Intelligence in Medicine, 124, 102256.
Liu, L., Zhou, R., Yuan, S., Sun, Z., Lu, X., Li, J., Chu, F., Walmsley, A. D., Yan, B., & Wang, L. (2022). AR navigation in implant dentistry based on CBCT-derived bone models: A pilot clinical study. International Journal of Computerized Dentistry, 25(1), 79-85.
Luongo, F., Zucchelli, G., Mazzotti, C., Mounajjed, R., Mazzotti, A., & Mazzotti, M. (2022). Augmented reality in dentistry: Uses and limitations of accessible technologies. Aesthetic Dentistry, 1(1), 30-35.
Kwon, H. B., Park, Y. S., & Han, J. S. (2023). Effectiveness of augmented reality-based learning in removable partial denture education: A randomized controlled study. Journal of Dental Education, 87(4), 459-467.
Pulijala, Y., Ma, M., Pears, M., Peebles, D., & Ayoub, A. (2021). An innovative virtual reality training tool for orthognathic surgery. International Journal of Oral and Maxillofacial Surgery, 47(9), 1199-1205.
Rahman, N., Wijesinghe, L., & Muthukumaraswamy, S. K. (2023). Faculty perceptions of augmented reality integration in dental education: A qualitative exploration. International Journal of Educational Research, 110, 101805.
Shah, N., & Pawar, A. (2022). Augmented reality in prosthodontics: The past, present, and future. International Journal of Prosthodontics, 35(1), 55-61.
Singh, R. P., Javaid, M., Kataria, R., Tyagi, M., Haleem, A., & Suman, R. (2022). Significant applications of virtual reality for the dentistry field in the COVID-19 era. Journal of Oral Biology and Craniofacial Research, 11(3), 407-413.
Wei, J., Chen, S., & Collins, C. (2024). Haptic feedback integration in dental AR systems: Current limitations and future directions. IEEE Transactions on Haptics, 17(1), 112-121.
Wijesinghe, L., Rahman, N., & Bencharit, S. (2023). Integration of digital scanning, CAD/CAM, 3D printing, and augmented reality in contemporary dental education. Journal of Dental Education, 87(3), 335-343.
Xiao, Z., Zhou, W., Zhang, N., & Zhou, Z. (2022). A comprehensive review of augmented reality in digital prosthodontics. Frontiers in Dental Medicine, 3, 786909.
Zhu, M., Liu, F., Chai, G., Pan, J. J., Jiang, T., Lin, L., Xin, Y., Zhang, Y., & Li, Q. (2021). A novel augmented reality system for displaying inferior alveolar nerve bundles in maxillofacial surgery. Scientific Reports, 7(1), 42365.
