Introduction
What is Autonomous Endodontic Robotics?
Autonomous endodontic robotics refers to robotic devices that can carry out endodontic tasks (like drilling an access cavity, cleaning canals, or performing root-end surgery) with a high degree of automation. Unlike standard dental instruments controlled entirely by the dentist, these robots use computer-guided motors and intelligent feedback to execute procedures according to a digital plan. In practice, an autonomous endodontic robot works by first using detailed images of the tooth (e.g. 3D scans from CBCT or optical scans) to plan the procedure. The plan – essentially a set of precise coordinates and movements – is loaded into the robot’s control system. During treatment, the robot’s arm positions and drives endodontic instruments (drills, files, etc.) along the planned path while monitoring position in real time. Advanced systems employ spatial alignment and registration methods to map the patient’s anatomy to the robot’s coordinate system (Locating a Calcified Root Canal with Robotic Assistance: A Case Report – Journal of Endodontics). This allows the robot to “know” exactly where the tooth and root canals are, even if the patient moves slightly or the target is not visible to the naked eye. Autonomous robots differ from simple static guides or manual instruments in that they can actively navigate and adjust motion on their own (within pre-set safety parameters), rather than just constraining a human operator. In endodontics, this means a robot could, for example, drill an access through a calcified canal or resect a root tip autonomously once the dentist programs the target location (Locating a Calcified Root Canal with Robotic Assistance: A Case Report – Journal of Endodontics). The dentist’s role shifts to preoperative planning, oversight, and handling any steps that the robot isn’t tasked with (like final obturation or decision-making for unexpected findings). Essentially, autonomous robotics in endodontics is about combining digital treatment planning with precise robotic execution to augment or automate the most technically demanding parts of a root canal or endodontic surgery.

Robotic Systems in Endodontic Procedures Today
Robotic applications in endodontics have quickly progressed from theory to reality in recent years. Several systems and prototypes are paving the way for robotic-assisted or fully automated endodontic treatments:

A utonomous Endodontic Microsurgery Robots (China): Pioneering work out of China has achieved true autonomy in endodontic surgery. In 2024, Liu et al. reported the first fully autonomous robot-assisted apicoectomy (root-end surgery) in a patient (Endodontic Microsurgery With an Autonomous Robotic System: A Clinical Report – PubMed). They planned a 3 mm apical resection on a molar using digital models, and the robot’s arm executed the cut precisely according to plan. The surgeon simply verified the result under the microscope afterward. No cracks or errors were found, and the procedure preserved more bone compared to manual techniques (Endodontic Microsurgery With an Autonomous Robotic System: A Clinical Report – PubMed). Building on that, in 2025 another team used a similar Autonomous Trajectory Robot (ATR) system to locate and remove a fractured file fragment protruding beyond a root tip
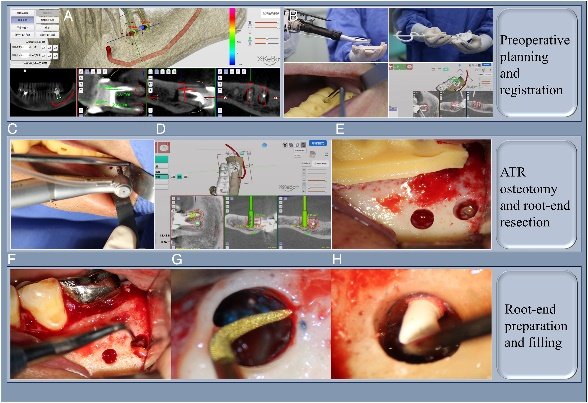
(Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text) (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text). The robot registered to the patient’s jaw, drilled a small “keyhole” access in the bone, and precisely guided itself to the metal fragment, allowing the surgeon to retrieve it with minimal bone removal. These cases highlight that autonomous robots can handle extremely fine endodontic tasks – drilling holes only a few millimeters in size at exact coordinates – with success. The calcified canal access is another striking example: Huang et al. (2025) reported a robot that autonomously drilled into a completely calcified upper incisor canal following a planned path, achieving access and relief of symptoms in a 49-year-old patient (Locating a Calcified Root Canal with Robotic Assistance: A Case Report – Journal of Endodontics) (Locating a Calcified Root Canal with Robotic Assistance: A Case Report – Journal of Endodontics). In all these cases, the robotic systems demonstrated sub-millimeter accuracy in targeting the root canal or apex while preserving critical structures like the cortical bone plate (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text).
E ndodontic Micro-Robot for Root Canals:
Beyond surgical applications, researchers have been designing robots to perform the entire sequence of root canal therapy automatically. A notable concept is the Columbia University “Advanced Endodontic Development” microrobot, first proposed by Hong and colleagues. This miniature robotic device would mount onto the patient’s teeth and carry out root canal treatment from start to finish (Robotics in the Contemporary Era of Conservative Dentistry and Endodontics – The Geek Chronicles). According to Dong et al. (2007) – who built a prototype – the system would use radiographs or a CBCT scan to generate a 3D model of the tooth, then a computer-aided prescription program plans the sequence of operations (Robotics in the Contemporary Era of Conservative Dentistry and Endodontics – The Geek Chronicles). The microrobot, clamped onto the tooth, would then automatically probe the canal, drill the access, clean the canal, and even fill it, all under continuous monitoring and intelligent control (Robotics in the Contemporary Era of Conservative Dentistry and Endodontics – The Geek Chronicles). The envisioned device is quite compact: about 2×2×2.8 cm, small enough to fit in the mouth and attach via a custom bracket on the target tooth () (). It contains micro-actuators to control a tiny drill/file with five degrees of freedom – essentially a “tiny CNC machine” for teeth () (). While still experimental, this microrobot represents the ambition to make root canal therapy a largely automated procedure in the future. Early prototypes validated the mechanical design and feasibility, but further work is needed on sensors and feedback to allow truly independent operation inside the canal system (Robotics in the Contemporary Era of Conservative Dentistry and Endodontics – The Geek Chronicles) ().
Haptic Training Simulators:

Another category of robotics in endodontics is not for patient treatment but for clinician training. Systems like the
OmniPhantom haptic virtual reality simulator
have been developed to help dentists practice root canal procedures in a virtual setting (
Robotics in the Contemporary Era of Conservative Dentistry and Endodontics – The Geek Chronicles). These devices use robotic haptic arms to simulate the feel of drilling into a tooth and negotiating canals. For example, Iranian researchers Toosi
et al.(2014) and Razaviet al(2015) created haptic-based endodontic training robots that provide force feedback as a trainee “instruments” a virtual canal (
Robotics in the Contemporary Era of Conservative Dentistry and Endodontics – The Geek Chronicles). Such simulators increase training efficacy by letting students experience realistic tactile resistance and even the sensation of a file catching, without risking a real tooth (
Robotics in the Contemporary Era of Conservative Dentistry and Endodontics – The Geek Chronicles). While not autonomous (they respond to the user’s movements), these systems incorporate robotic technology to improve endodontic education and ultimately enhance practitioners’ skills in using the real autonomous systems.
Microrobotic Swarms for Cleaning:

A very different approach to robotics in endodontics involves
microscale robots
that can move inside the canals themselves. Researchers at the University of Pennsylvania (CIPD center) have demonstrated magnetically controlled iron-oxide nanoparticle swarms that act as tiny robots to clean and disinfect canal walls (
Penn Dental Medicine Study Applies Microrobotics in Endodontic Treatment, Diagnostics – Penn Dental Medicine). In a 2022 proof-of-concept, they showed that these microrobots can be guided throughout the complex internal anatomy of a root canal,
disrupting biofilms and even retrieving samples
for diagnostic analysis (
Penn Dental Medicine Study Applies Microrobotics in Endodontic Treatment, Diagnostics – Penn Dental Medicine) (
Penn Dental Medicine Study Applies Microrobotics in Endodontic Treatment, Diagnostics – Penn Dental Medicine). One platform uses a magnetic field to concentrate nanoparticles into moving “microswarm” brushes that scour the canal surfaces; another uses 3D-printed helical microrobots (like tiny screws) that carry antimicrobial agents to specific sites (
Penn Dental Medicine Study Applies Microrobotics in Endodontic Treatment, Diagnostics – Penn Dental Medicine). Though these are on the research bench for now, the vision is to integrate microrobots into endodontic treatment so that after mechanical instrumentation, a swarm of microrobots could navigate into fins, isthmuses, and lateral canals to thoroughly disinfect areas traditional tools and irrigants might miss (
Applying Microrobotics in Endodontic Treatment and Diagnostics – Penn Engineering Blog). This would greatly reduce residual bacteria and improve root canal success rates. Microrobotic therapy might one day be the companion to a macro-scale robotic arm, together achieving a truly automated and optimally cleaned root canal.
(Applying Microrobotics in Endodontic Treatment and Diagnostics – Penn Engineering Blog) Cone-beam CT images showing a magnetically guided microrobot (red arrows) precisely reaching the apical region of a root canal. In a Penn Dental Medicine study, such microrobots successfully navigated complex canal spaces to disrupt biofilm and aid disinfection (Applying Microrobotics in Endodontic Treatment and Diagnostics – Penn Engineering Blog).
Integration of AI, Imaging, and Real-Time Navigation
A key enabler of autonomous robotics in endodontics is the integration of advanced imaging and artificial intelligence for planning and guidance. High-resolution imaging is the foundation: Cone-Beam CT (CBCT) scans provide a 3D map of the tooth’s internal anatomy, including canal shapes and surrounding bone. Some new robots even use optical coherence tomography (OCT) to scan teeth with light, avoiding radiation and automatically detecting structural details like cavities or calcifications with AI analysis (Fully-automatic robot dentist performs world’s first human procedure) (Fully-automatic robot dentist performs world’s first human procedure). Once a 3D model of the tooth is obtained, intelligent software can plan the optimal path for intervention. For example, in robotic endodontic microsurgery cases, the dentist (with software assistance) chooses a target point on the root and the software calculates the trajectory and depth for drilling to that target (Locating a Calcified Root Canal with Robotic Assistance: A Case Report – Journal of Endodontics). AI algorithms can assist by analyzing the scan to identify the canal or lesion location and suggesting the safest, least invasive path – essentially automated treatment planning (). This is akin to CAD/CAM in other fields: the plan might specify where the robot should enter the tooth, at what angle, and how deep to drill, taking into account the patient’s unique anatomy.
During the procedure itself, real-time navigation and feedback are critical. Robotic systems use a variety of methods to ensure the execution stays true to the plan. One common approach is to employ optical or physical registration markers so the robot knows its position relative to the patient. In the autonomous cases from China, they incorporated intraoral reference markers and performed a spatial alignment (registration) of the robot’s coordinate system to the patient’s jaw using the pre-op scan (Locating a Calcified Root Canal with Robotic Assistance: A Case Report – Journal of Endodontics) (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text). This allowed the robot arm to move to the correct location even though the patient’s anatomy is never identical to the scan (minor positioning differences are corrected by the registration). As the robot operates, sensors provide live feedback: encoders track the drill bit position, and imaging can be used to confirm progress. For instance, the ATR robot displays the drill’s position on the CBCT image in real time during osteotomy, giving the surgeon visual confirmation of the depth and angle being achieved (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text). Haptic feedback is another safety layer – in a system like Yomi, the robot applies physical resistance if the dentist tries to move off the planned path, effectively preventing deviation or excessive drilling (Robot demonstrates dental implant procedures – UBNow: News and views for UB faculty and staff – University at Buffalo) (Robot demonstrates dental implant procedures – UBNow: News and views for UB faculty and staff – University at Buffalo). Some robots have force sensors to detect increased resistance (e.g., if a drill is pressing too hard or a file is binding) and can pause or adjust accordingly to avoid file breakage or perforation.
Artificial intelligence (AI) further enhances these capabilities by enabling adaptive decision-making. AI image analysis can automatically locate canal orifices or calcifications on scans that might be hard for human eyes to spot (The Orchestrated Future: AI’s Impact on Precision in Endodontic Consumables | by Sneha | Medium) (The Orchestrated Future: AI’s Impact on Precision in Endodontic Consumables | by Sneha | Medium). During treatment, AI could monitor sensor data (force, torque, etc.) and recognize patterns – for example, detecting the subtle change in vibration that precedes a file separation and then stopping the robot before it happens. In the near future, we may see AI-driven control systems that allow the robot to adjust its plan on the fly if conditions change (such as the canal taking an unexpected curvature) (). For now, most robotic endodontic systems still rely on predetermined instructions, but even these benefit from AI at the planning stage. An AI algorithm can sift through a large database of past cases to suggest an optimal approach for a given tooth anatomy, essentially serving as a “digital endodontic expert” to guide the robot. The combination of precise imaging, real-time tracking, and AI decision support creates a closed-loop system: plan, execute, monitor, and adjust. This integration is what makes it possible for a robot to navigate the intricate maze of a root canal system without straying, ensuring that the procedure remains on target and as minimally invasive as possible (Locating a Calcified Root Canal with Robotic Assistance: A Case Report – Journal of Endodontics). In essence, imaging provides the eyes, AI provides the brain, and robotics provides the steady hands for a new era of endodontic precision.
Benefits of Robotic Assistance in Endodontics
Adopting autonomous or semi-autonomous robots for complex endodontic procedures offers several significant benefits over purely manual techniques:
- Unmatched Precision and Accuracy: Robots can execute movements at a sub-millimeter scale with perfect repeatability. This level of precision reduces the risk of missing tiny canals or deviating from the ideal path. For example, robotic assistance enabled perfectly targeted access to a calcified canal and precise removal of a 7 mm broken file segment, all while avoiding excessive removal of tooth or bone (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text). Studies have indicated that robotic-guided endodontics can improve the success rate of treatments by ensuring canals are thoroughly treated without iatrogenic errors (). The robot’s steady hand and constant feedback essentially eliminate human hand tremor and guesswork from critical steps.
- Minimally Invasive Access: Because of their accuracy, robots allow clinicians to take a more conservative approach. A robot can create a very small osteotomy or access cavity that is just big enough for the task, preserving healthy tooth structure and bone. In the autonomous apicoectomy cases, the cortical plate was kept intact except for a precise 3 mm osteotomy, something hard to achieve freehand (Endodontic Microsurgery With an Autonomous Robotic System: A Clinical Report – PubMed). This minimally invasive approach promotes quicker healing and less postoperative discomfort. The ability to consistently find calcified canals with pinpoint accuracy means avoiding the large exploratory drilling that can significantly weaken teeth.
- Reduced Operator Fatigue and Improved Ergonomics: Endodontic procedures often require intense focus and awkward hand positions under a microscope for extended periods. Robotic systems can take over the strenuous parts of the procedure (like continuous drilling or filing), sparing the dentist from prolonged repetitive motions. By offloading these tasks, robots help alleviate physical strain on practitioners, which can maintain their performance over long procedures (). A dentist operating a robot often works in a more natural posture (perhaps seated at a console or just supervising), rather than hunching over the patient. In the long run, this could reduce work-related musculoskeletal issues and extend careers.
- Consistency and Reproducibility: Every patient’s anatomy is unique, but robots follow their programmed instructions exactly each time. This means that outcomes become more predictable. A properly calibrated robot will drill to precisely the intended depth – no more, no less – across different patients, eliminating variability. This consistency is crucial in complex cases; even a highly experienced endodontist may have slight differences day to day, but a robot does not fatigue or get distracted. Robotic procedures have shown more predictable results in complex anatomy compared to manual techniques (). This reliability can translate to higher overall success rates, especially for challenging anatomies or re-treatments that traditionally have variable outcomes.
- Enhanced Safety and Avoidance of Errors: Many potential mishaps in endodontics (perforating the root, over-drilling into bone, breaking instruments) are due to human error or limitations. Robots can be programmed with safety boundaries – for instance, not to drill beyond a certain depth or outside a planned angle – effectively creating an error-proof system. In a haptic-guided setup like Yomi, the robot will not allow the dentist to make a critical mistake such as drilling past the root tip into vital structures (Robot demonstrates dental implant procedures – UBNow: News and views for UB faculty and staff – University at Buffalo). If any discrepancy from the plan occurs (like a calibration issue or sudden obstruction), the system can halt and alert the operator. Additionally, by integrating with real-time imaging or tracking, robots can automatically compensate for patient movement, maintaining safety in situations that might otherwise lead to off-target drilling. The net effect is a significant reduction in complications like perforations, nerve injuries, or missed canals. One could say the robot “shares its pro level precision” with every dentist using it, raising the floor for the standard of care.
- Shorter Procedure Times (in some cases): Although setup and planning with a robot take time, the actual execution of tasks can be faster than manual performance. Robots don’t need breaks and can work efficiently once engaged. In one report, an autonomous dental robot prepared a crown in about 15 minutes, whereas a human would take closer to 2 hours (Fully-automatic robot dentist performs world’s first human procedure). In endodontics, if a robot can rapidly create an access cavity or perform canal preparation in a streamlined way, it could shorten the overall appointment. By automating repetitive steps (like continuous drilling of a calcified canal), the robot frees the clinician to perform other tasks in parallel or simply finish the procedure sooner. It should be noted that current endo robots are still in early stages, and not all studies show time savings (sometimes setup can offset it). But as the technology improves, efficient robotic workflows are expected to reduce chair time without compromising quality () – a win-win for patient and provider.
In summary, robotic assistance introduces a new level of control and accuracy to endodontics, translating to better outcomes (more complete debridement and filling), fewer mistakes, and a more comfortable experience for both patient and dentist. Especially in anatomically or technically difficult cases, these benefits become most pronounced – a robot doesn’t mind if a canal is S-shaped or the tooth is hard to reach, it will perform with the same precision regardless.
Case Studies and Clinical Evidence
Robotic endodontics is moving from concept to clinic, with a growing number of case studies and trials demonstrating its real-world feasibility. Below are a few landmark examples that highlight successful implementation of robotics in complex endodontic procedures:
Robot-Guided Apicoectomy (Root-End Surgery): Chen Liu and colleagues (2024) documented the first-ever use of an autonomous robot to perform an apicoectomy on a lower molar (Endodontic Microsurgery With an Autonomous Robotic System: A Clinical Report – PubMed). In this case, the patient had a persistent infection at the root tip. A surgical plan was created on software, and the robot was registered to the jaw using the patient’s CT data. The robot’s arm then autonomously drilled a 3 mm diameter osteotomy and resected the infected root tip with sub-millimeter accuracy (Endodontic Microsurgery With an Autonomous Robotic System: A Clinical Report – PubMed) (Endodontic Microsurgery With an Autonomous Robotic System: A Clinical Report – PubMed). The endodontist only took over to do the retrograde filling under the microscope after the robot had finished the bone cut. The result was a perfectly executed root resection without complications. The authors noted this could minimize errors from operator inexperience and avoid removing more bone than necessary, since the robot cut exactly what was planned (Endodontic Microsurgery With an Autonomous Robotic System: A Clinical Report – PubMed). This case is a milestone showing that autonomous robots can successfully handle the delicate bony surgery aspect of endodontics.
Haptic Robot-Assisted Endodontic Surgery:
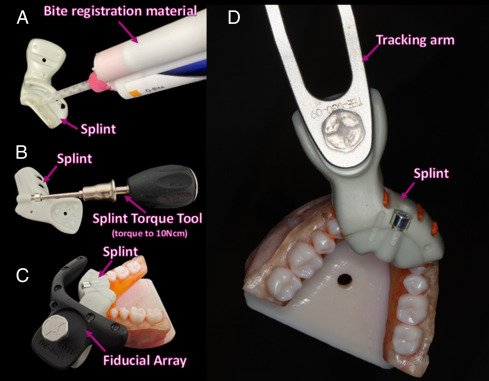
Another case report (Isufi
et al., 2024) used the Yomi robotic system in a
robot-assisted apicoectomy on two upper premolars(
Robot-Assisted and Haptic-Guided Endodontic Surgery: A Case Report – PubMed). Unlike the fully autonomous example above, Yomi provides “active guidance” while the surgeon performs the motions. In this case, after planning the apical surgeries on a CBCT scan, the Yomi robot guided the surgeon’s handpiece for the osteotomy and root-end cuts. It provided real-time feedback and physically kept the burr on the correct trajectory (
Robot-Assisted and Haptic-Guided Endodontic Surgery: A Case Report – PubMed). The report concluded that the introduction of this technology in endodontics was promising and could enhance precision and reduce human error. It effectively functioned as a smart drill guide that the patient can’t dislodge and that adapts to the tooth’s position in 3D space. The significance is that even current commercial dental robots (designed for implants) have immediate utility in endodontics when used in this semi-autonomous mode, indicating a shorter learning curve and faster adoption for clinicians (
Emerging robot-guided techniques in endodontic microsurgery – LWW) (
Robot demonstrates dental
Removal of a Fractured Instrument via Robot (ATR System):
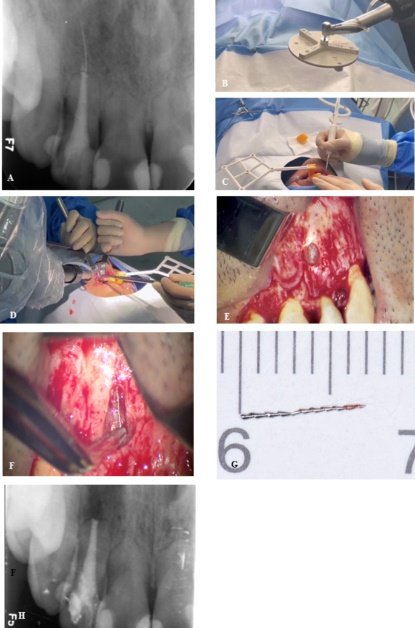
File breakage inside canals is a dreaded complication. Fu et al. (2025) tackled a case with a broken file segment that had extruded past the root tip, requiring surgical removal (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text) (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text). Using the Autonomous Trajectory Robot (ATR) system, they planned a conservative surgical approach. The robot was registered and guided to create a tiny round bone window right over the fragment’s tip. It then independently positioned a drill to exactly the location of the fragment beyond the apex, allowing the surgeons to retrieve the fragment through the small access (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text) (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text). Impressively, the procedure preserved all cortical bone and the total robot drilling time was only 9 minutes (after about 30 minutes of setup) (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text). At 9-month follow-up the lesion had healed with bone fill. The conclusion was that the ATR enabled precise localization and removal of the broken file with minimal invasiveness and reduced operating time (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text). This case demonstrates the robot’s ability to perform delicate microsurgery (removing just the right amount of bone to get an object out) far better than freehand surgery could.
In Vitro and Ongoing Trials: Beyond individual cases, laboratory studies and pilot trials are underway. One in vitro study compared the accuracy and operation time of robotic endodontic microsurgery vs. dynamic navigation vs. traditional surgery (Endodontic Microsurgery With an Autonomous Robotic System: A Clinical Report – PubMed). Early results indicate the robot-guided approach can achieve equal or better accuracy than even the modern dynamic navigation systems, though refinement is needed to reduce setup time. There are also ongoing efforts to use robots for guided endodontic access in teeth with challenging anatomies (like dens invaginatus or oddly angulated roots), which traditionally use 3D printed guides. A robot could add more flexibility and precision than a static guide. Clinical trials are still in very early phases – we’re mostly seeing case reports (level 4 evidence) at this point – but the consistency of positive outcomes in these reports is building confidence. Each success – from basic access cavities to apical surgeries – lays the groundwork for larger studies. In the coming years, we expect formal clinical trials to evaluate robotic vs. conventional endodontic outcomes in terms of success rates, patient pain, procedure time, etc., providing the data needed for regulatory approvals and broader adoption.
Together, these case studies illustrate that robotic systems are already capable of handling some of the most difficult endodontic scenarios. From finding invisible canals to precisely resecting root apices and removing obturation mishaps, robots have shown they can do it all with finesse. The learning from these early cases is guiding improvements in the technology – for example, better user interfaces, faster registration methods, and more compact robotic arms to fit in the mouth. As more clinicians gain access to these systems (often via academic centers or experimental programs), the pool of expertise and comfort with robotic endodontics will grow, likely accelerating more widespread use.
Limitations and Challenges
Despite the exciting potential, autonomous robotics in endodontics comes with several limitations and challenges that must be addressed as the technology evolves:
- High Cost and Accessibility: Robotic systems are expensive to develop, purchase, and maintain. A full dental robotic setup can be a significant capital investment, which currently limits availability to large specialty clinics or research institutions. The initial cost and upkeep (calibration, servicing, software updates) create a barrier for many private practices () (). In developing regions or small clinics, these costs may be prohibitive, meaning robotic endodontics could remain confined to high-resource settings initially () (). As the technology matures, costs may come down, but demonstrating clear return on investment (through improved outcomes or efficiency) will be key for adoption.
- Technical Complexity and Learning Curve: Introducing robots into endodontic practice is not plug-and-play. Dentists must learn to operate the software for planning and the robot hardware. This requires training in areas not traditionally taught in dental school (imaging software manipulation, interpreting 3D plans, managing robotic interfaces). There can be a steep learning curve to use these systems effectively (). Practitioners comfortable with freehand techniques might be hesitant to trust and rely on a machine initially. Additionally, workflow integration is a challenge – incorporating the scanning, planning, and robot setup into a normal clinic schedule can be cumbersome until proficiency is achieved. User-friendly design and good training programs will be crucial to lower this barrier.
- Current Robots are Not Fully Autonomous (Yet): Ironically, while we use the term “autonomous robotics,” most commercially available dental robots are still semi-autonomous or require continuous human oversight. Systems like Yomi require the dentist’s hand on the handpiece; even the ATR cases involved the dentist initiating actions (stepping on a pedal to start drilling, etc.) (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text) (Removal of a fractured file beyond the apical foramen using robot-assisted endodontic microsurgery: a clinical report | BMC Oral Health | Full Text). In other words, these robots don’t make independent clinical decisions – they follow a pre-set plan. This means the dentist is still responsible for monitoring and adjusting if something isn’t going as expected. If the robot encounters an unforeseen scenario (like an unusual resistance or anatomic variant outside the plan), it typically stops and waits for human input. So at the present stage, robots enhance precision but do not replace the need for an attentive endodontist at the helm () (). Over time, as AI improves, we may see more “decision-making” autonomy, but for now the limitation is that these are sophisticated assistive tools rather than entirely independent surgeons.
- Size and Access Limitations: Working in the mouth is tricky for any device – there’s limited space to accommodate tools. Many robotic arms are relatively large (adapted from industrial or surgical robots). Fitting the arm and handpiece into a small oral opening, especially for posterior teeth, can be challenging. In some cases, patients with limited mouth opening or strong gag reflex might not tolerate the hardware. Efforts are underway to create more compact robots and even intraoral robots (like the micro-robot concept), but currently the bulkiness of equipment is a consideration. There’s also the need for line-of-sight or reference markers – sometimes a stent or fiducial marker must be attached to the teeth for registration, which is an extra object in the mouth to manage () (). These practical issues must be refined to make robotic endodontics seamless.
- Patient Acceptance and Trust: Dental anxiety is common, and some patients might be even more nervous about a “robot” performing their root canal. Gaining patient acceptance is an important hurdle. In early surveys and anecdotal reports, some patients express hesitation to be treated by a machine, preferring the perceived assurance of a human touch (Robotics in the Contemporary Era of Conservative Dentistry and Endodontics – The Geek Chronicles). Clear communication will be needed to explain that the dentist is still in control and the robot is a precise instrument to help them. Interestingly, the flip side also exists – certain tech-savvy patients are intrigued by advanced technology and may actually seek out robotic-assisted care, thinking it superior. Broadly, though, public trust in autonomous medical procedures is still developing. Ensuring a track record of safety and positive outcomes will gradually build confidence. It’s worth noting that as robotic surgery (like Da Vinci robots) has become more common in medicine, patient acceptance has grown; a similar trend may happen in dentistry with time.
- Ethical and Legal Considerations: The introduction of autonomy raises questions of responsibility and ethics. For instance, if a robotic system makes an error that harms a patient, who is liable – the dentist operating it, the manufacturer, or the software algorithm? Clear guidelines and regulations will be needed to define accountability (). There are also concerns about data security (the digital models and plans are patient data that need protection) and the ethical implications of machine decision-making in healthcare. Informed consent documents may need to explicitly mention robotic assistance. Regulatory bodies (like the FDA) will scrutinize autonomous dental devices for safety and efficacy, which means robust clinical evidence is needed for approvals. Additionally, widespread automation brings up the ethical debate of how much we should rely on machines – dentistry is as much art as science, and some worry that over-reliance on robots could deskill practitioners over time. Balancing innovation with professional skill and patient autonomy (patients have the right to refuse robotic treatment if uncomfortable) will be an ongoing dialogue.
- Integration with Existing Practice: From a practical standpoint, clinics will have to adapt their infrastructure to accommodate robots. This might mean longer appointment slots initially, new scheduling considerations, and coordination between imaging departments and operative dentistry. Dental assistants and support staff will need training to assist in robotic procedures (for example, managing the software or positioning the robot). There may be resistance to change in well-established practices. Showing that robotic procedures can fit into a normal clinic day without undue disruption is part of the challenge. As the technology improves (for instance, faster automated registration or easier setup), these integration issues will lessen.
In summary, while the promise of robotic endodontics is high, there are real-world hurdles to overcome. Cost, complexity, and cautious attitudes are natural at this early stage. The good news is that each successful case and each improvement in the technology is actively addressing these challenges. The trajectory often seen in medical robotics is playing out here too – initial systems are expensive and somewhat clunky, but successive iterations become more affordable and user-friendly, and as clinicians get more comfortable, adoption grows. Addressing training and safety through proper guidelines will ensure that as we overcome the limitations, robotic endodontics is implemented in an ethical, patient-centered manner.
Future Trends and Outlook
Looking ahead, the field of robotic endodontics is poised for significant advancements that could make autonomous robots a routine part of dental care. Here are some future trends and how robotics may evolve in endodontics:
Deeper AI Integration: Artificial intelligence will play an increasingly central role in robotic endodontic systems. In the future, we can expect AI to handle more of the decision-making – for instance, analyzing a patient’s scan and not only planning the procedure but also predicting possible complications (like a likely ledge formation or risk of perforation) (). Machine learning models trained on thousands of cases could provide real-time guidance to the robot, allowing it to adjust mid-procedure. This could lead to fully autonomous root canal procedures where the robot can adapt to what it “feels” or “sees” in the canal (through sensors), much like an experienced dentist would. The AI would continuously learn from each case, improving the robot’s performance over time. Such adaptive robots might one day handle an entire root canal while the dentist observes – an extension of the concepts proven by the current ATR systems.
Enhanced Imaging and Navigation: We will likely see more use of non-ionizing, high-speed imaging like OCT for intraoperative guidance, as demonstrated by the Perceptive robotic system for cavity preparation (Fully-automatic robot dentist performs world’s first human procedure). Imagine a robot that can perform a quick scan inside a canal during treatment to see how much debris remains, then decide to brush that area a bit more – all in seconds. Real-time 3D imaging feedback could make robotic endodontics extremely precise. Additionally, better navigation technology (perhaps miniaturized scanners that fit in the mouth) will simplify the registration process. We might get to a point where the patient bites on a sensor and the robot instantly knows its position relative to the tooth, cutting setup time dramatically. These improvements in navigation will also enable teleoperated endodontics – a specialist could remotely plan and even oversee a robot performing a root canal in a rural clinic, given high-fidelity data streaming and control interfaces.
3D Printing & Custom Tool Integration: The synergy between 3D printing and robotics will likely grow. We could see customized endodontic instruments or guides being printed on the fly for a specific case, and the robot using those for optimal results (). For example, a personalized drill bit angle or a shaped file that exactly matches a patient’s canal curvature could be fabricated and then the robot is programmed to use it. This customization would further increase efficiency and success rates. 3D-printed attachments might also help robots reach difficult areas – such as a printed extension that lets a robotic arm work around a limited jaw opening. Essentially, patient-specific tooling enabled by 3D printing can be combined with robotic delivery for truly individualized care ().
Microscale Robots and Swarm Tech: The microrobotics discussed earlier will likely mature and possibly integrate with macro-robots. In the future, an endodontic appointment might involve a two-phase robotic approach: a larger robot does the access and gross cleaning, then deploys a swarm of microscale robots into the canal system for final disinfection and even obturation. These microrobots could be designed to degrade and flush out after completing their task, or be magnetically extracted. Research is also ongoing into nano-robots that could deliver medications or even promote healing at the apical area after a root canal (Penn Dental Medicine Study Applies Microrobotics in Endodontic Treatment, Diagnostics – Penn Dental Medicine) (Penn Dental Medicine Study Applies Microrobotics in Endodontic Treatment, Diagnostics – Penn Dental Medicine). Such innovations could significantly improve healing and reduce post-treatment complications. It’s conceivable that one day a root canal might be done with almost no traditional files or sealers – instead, a robot bores a small access, and injectable robots clean out pulp tissue and bacteria, then perhaps solidify into a sealant to fill the canal.
Portability and Miniaturization: Current robotic units are fairly large, often occupying a significant footprint in the operatory. Future designs aim to be more compact or even portable. Researchers anticipate compact robotic systems that could be moved between operatories or even clinics, broadening access () (). Some concepts involve robots that attach directly to the patient (as we saw with the micro-robot mounted on teeth) which would eliminate the need for a big external arm. As components get smaller (thanks to advancements in motors, batteries, etc.), we might see robots the size of a handheld device that can perform automated endodontics. Imagine a device that a dentist clips onto a tooth and it performs the root canal while attached – this is essentially the Columbia micro-robot vision, and it could become reality with future engineering refinements.
C ollaborative Robotics (Cobots):

The future likely isn’t an “all or nothing” of either dentist or robot – it will be collaboration between human and machine. The concept of “cobots” (collaborative robots) involves robots designed to work in tandem with clinicians (). In endodontics, a cobot might intelligently adjust to the dentist’s motions – for instance, if the dentist is manually negotiating a tricky canal, the cobot could steady their hand or limit the range so they don’t perforate. This approach can provide a balance: the dentist retains decision-making and tactile feel, while the robot provides stability, memory (holding a position), or executing tedious parts. Cobots could also handle auxiliary tasks like irrigation or holding suction in the perfect spot, which frees up the dentist and assistant to focus on critical steps (). By working side by side, overall efficiency and safety improve without fully handing over control. This kind of human-robot teamwork is very much expected in dental clinics of the future.
Greater Adoption and Skill Development: As robotics become more common, dental education will evolve. We’ll likely see training on robotic systems incorporated into endodontic residency programs, so new specialists come out ready to use these tools. Over the next decade, what is novel today (like using a robot for an apicoectomy) may become a standard option, especially for difficult cases. Manufacturers are actively improving the user experience, making interfaces more intuitive and shortening the learning phase. If clinical trials continue to show positive results – e.g., higher success in retreatments or less post-op pain due to minimal bone removal – evidence-based guidelines might eventually recommend robotic assistance for certain procedures. With time, patient perceptions will also shift: a generation growing up with technology may feel more comfortable knowing a precise robot (overseen by a skilled dentist) is involved in their care.
In conclusion, the trajectory of autonomous robotics in endodontics is very promising. What started as bold ideas in research labs is now already saving teeth in the clinic. In the near future, we can expect robots to become smarter, smaller, and more integrated into everyday endodontic practice. They will not replace endodontists – rather, they will amplify the capabilities of clinicians, allowing us to tackle cases that were previously deemed hopeless or too risky. Robotic endodontics is set to transform the landscape of dental care by enhancing precision, safety, and efficiency (), ultimately improving outcomes for patients with complex endodontic needs. The drill of the future may very well be a robot’s arm – guided by the mind of an endodontist and the intelligence of AI – working in harmony to preserve natural teeth with unparalleled accuracy.
