Subtitle: Advanced Digital Techniques and Material Selection for Predictable Cosmetic Outcomes
Keywords: midline diastema, aesthetic restorations, cosmetic prosthodontics, direct composite, porcelain veneers, digital smile design, minimally invasive dentistry, diastema closure, anterior esthetics
Executive Summary
This comprehensive review addresses the clinical management of maxillary midline diastemas through contemporary aesthetic restorative approaches. Midline diastemas, defined as spaces exceeding 0.5mm between the maxillary central incisors, present both aesthetic concerns for patients and unique clinical challenges for dental practitioners. This article examines current evidence-based protocols for diastema management, focusing on the spectrum of treatment options from minimally invasive direct composite techniques to comprehensive porcelain veneer solutions. Digital advancements in treatment planning, particularly digital smile design and CAD/CAM applications, have revolutionized diagnostic capabilities and predictability in diastema closure cases. Material selection criteria are analyzed based on case-specific requirements, with contemporary composite systems and ceramic materials compared for their optical properties, biomechanical characteristics, and long-term clinical performance. Special attention is given to emerging technologies that enable ultra-conservative preparations while maximizing aesthetic outcomes. The article provides detailed case presentations demonstrating successful implementation of these principles across varying diastema widths and clinical complexities. For dental practitioners seeking to optimize aesthetic outcomes while preserving tooth structure, this article offers actionable protocols for comprehensive assessment, digital planning, and technical execution of diastema closure cases using the latest materials and techniques in cosmetic prosthodontics.
1. Introduction & Background
Maxillary midline diastemas represent one of the most common aesthetic concerns that prompt patients to seek cosmetic dental treatment. While cultural perceptions of diastemas vary—considered attractive in some societies and undesirable in others—research by Rosenstiel et al. (2021) indicates that in Western populations, spaces exceeding 0.5mm between maxillary central incisors are generally perceived as aesthetically compromising by both patients and observers.
Historically, midline diastemas were managed through conventional crown preparations or orthodontic approaches, often resulting in unnecessary tooth structure removal or extended treatment timelines. The evolution of adhesive dentistry, coupled with advancements in biomaterials and digital technologies, has transformed the management of diastemas toward more conservative and predictable approaches.
The etiology of midline diastemas is multifactorial, including:
- Developmental factors (tooth-size discrepancies, microdontia)
- Anatomical variations (abnormal frenal attachments, missing lateral incisors)
- Pathological conditions (periodontal disease with tooth migration)
- Habitual behaviors (tongue thrusting, digit sucking)
- Skeletal discrepancies (maxillary-mandibular disharmony)
Understanding the underlying cause is crucial for treatment planning, as failure to address etiological factors can result in diastema recurrence. Contemporary management strategies have evolved beyond simple space closure to encompass comprehensive aesthetic analysis, including tooth proportions, gingival architecture, and dynamic smile elements.
This article aims to provide clinicians with evidence-based guidelines for managing midline diastemas through aesthetic restorative approaches, utilizing both traditional techniques and emerging digital technologies to achieve optimal functional and aesthetic outcomes while preserving tooth structure.
2. Clinical/Technical Overview
A. Comprehensive Diagnostic Assessment
Before initiating treatment for midline diastemas, a structured diagnostic approach is essential:
- Aesthetic Analysis
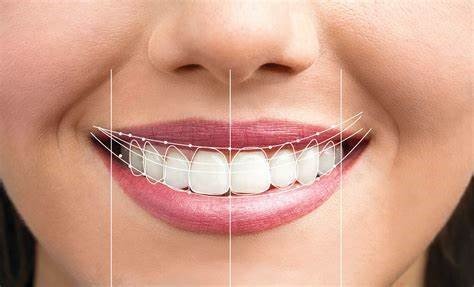
- Digital Smile Design Protocol
- Facial reference lines (interpupillary, commissural lines)
- Golden proportion assessment (ideal width-to-length ratio: 75-80%)
- Dental midline evaluation relative to facial midline (deviations <2mm generally acceptable)
- Gingival zenith positions and symmetry
- Incisal edge position and anterior guidance evaluation
- Occlusal Analysis

- Dynamic Occlusal Considerations
- Anterior guidance patterns
- Envelope of function
- Parafunctional risk assessment
- Occlusal stability evaluation
- Space Analysis

- Diastema Characterization
- Width measurement (mm)
- Tooth size analysis (Bolton analysis)
- Black triangle risk assessment
- Root proximity evaluation
- Etiological Assessment
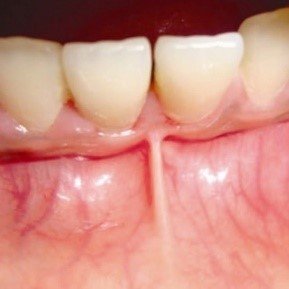
- Contributing Factors Identification
- Frenal attachment examination
- Skeletal relationship analysis
- Periodontal status evaluation
- Tongue posture and function assessment
B. Treatment Planning Considerations
The decision matrix for selecting appropriate treatment modalities depends on several factors:
| Clinical Parameter | Direct Composite Indication | Porcelain Veneer Indication | Digital Consideration |
| Diastema Width | <2mm | >2mm | Digital wax-up for proportional analysis |
| Tooth Position | Minimal rotation | Moderate-severe rotation | Digital articulation simulation |
| Color Change Needed | Minimal-moderate | Moderate-significant | Digital shade mapping and simulation |
| Existing Restorations | None/minimal | Moderate-extensive | Digital integration with existing restorations |
| Occlusal Forces | Normal | Heavy/parafunctional | Digital occlusal analysis |
| Treatment Timeframe | Immediate-short term | Multiple appointments | Digital treatment visualization |
| Patient Age | Younger patients | Adult patients | Age-appropriate digital simulations |
| Budget Considerations | Limited | Flexible | Digital cost-benefit visualization |
C. Material Selection Science
The biomechanical and optical properties of restorative materials significantly impact diastema closure outcomes:
1. Direct Composite Systems
- Nano-hybrid Composites

- Particle size: 0.005-0.01μm
- Flexural strength: 120-160 MPa
- Ideal for anterior restorations due to high polishability and color stability
- Examples: 3M Filtek Supreme Ultra, Tokuyama Estelite Sigma Quick
- Nano-ceramic Composites

- Enhanced wear resistance (30-40% improvement over conventional composites)
- Chameleon effect for superior blending
- Examples: GC G-ænial Universal Injectable, Kerr Harmonize
2. Indirect Ceramic Materials
- Lithium Disilicate

- Flexural strength: 360-400 MPa
- Excellent optical properties (translucency: 21-29%)
- Minimal preparation requirements (0.3-0.5mm)
- Examples: IPS e.max Press, Initial LiSi Press
- Feldspathic Porcelain
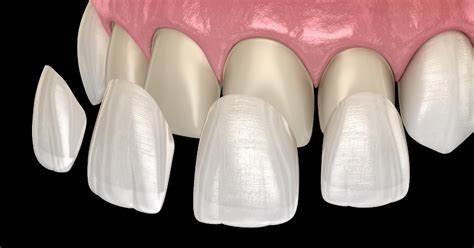
- Superior aesthetics with natural light transmission
- Flexural strength: 90-120 MPa
- Ultra-thin applications possible (0.2-0.3mm)
- Examples: VITA VM13, Creation CC
- Zirconia-Reinforced Lithium Silicate

- Hybrid strength and aesthetics
- Flexural strength: 420-450 MPa
- CAD/CAM optimized materials
- Examples: VITA Suprinity, Celtra Duo
D. Digital Workflow Integration
Contemporary diastema management increasingly incorporates digital technologies:
- Digital Impression Systems
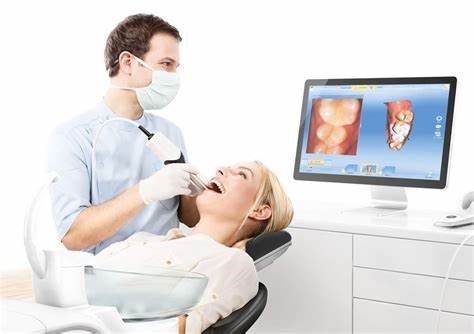
- Intraoral scanning accuracy for anterior teeth: 6-12μm deviation
- Real-time visualization and immediate assessment
- Integration with digital smile design software
- Popular systems: iTero Element 5D, Trios 4, Primescan
2. Digital Smile Design Software
- 2D and 3D smile simulations
- Digital wax-up capabilities
- Precise proportion analysis
- Leading platforms: DSD App, Smile Designer Pro, exocad Smile Creator
- CAD/CAM Integration

- Direct design of restorations
- Milling precision for veneers: ±25μm
- Immediate provisional fabrication capability
- Chairside systems: CEREC Primescan, Planmeca FIT
- 3D Printing Applications
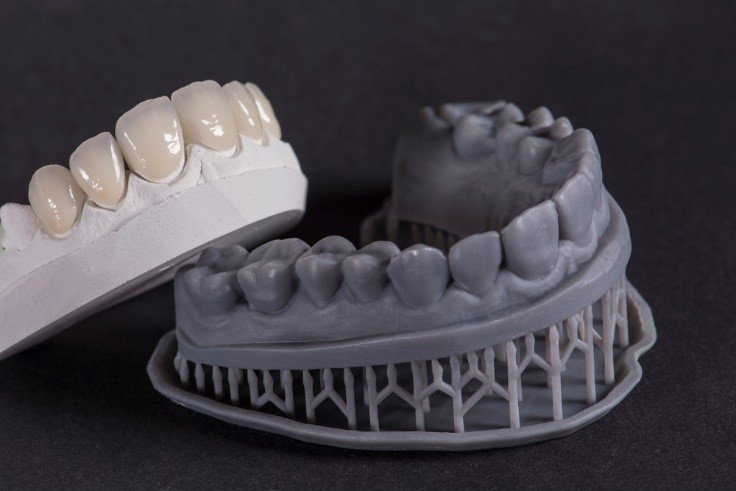
- Diagnostic mock-up printing
- Preparation guides and reduction indexes
- Provisional restoration fabrication
- Materials: BioMed Amber, KeySplint Soft Clear
3. Case Studies & Clinical Applications
Case Study 1: Minimally Invasive Direct Composite Approach
Patient Profile:
- 28-year-old female
- Chief complaint: “I’m embarrassed to smile because of the gap between my front teeth”
- 1.8mm midline diastema
- No previous restorations
- High aesthetic expectations with limited budget
Diagnostic Findings:
- Normal frenal attachment
- Ideal tooth proportions aside from diastema
- No occlusal interferences
- Mild tooth rotations (<5°)
Treatment Approach:
- Digital smile design simulation to visualize outcome
- Shade selection: A1 body with incisal translucency
- No preparation approach with selective enamel etching
- Silicon palatal index fabrication from digital mock-up
- Layer-by-layer composite application:
- Palatal shell: A1E enamel shade (0.5mm thickness)
- Dentin core: A1D dentin shade
- Incisal effects: Blue-white characterization
- Final enamel layer: A1E with 0.3mm thickness
- Finishing and polishing protocol:
- Contouring with fine diamonds (30μm grit)
- Multi-step polishing system (Sof-Lex discs)
- Final polish with diamond paste (0.5μm)
One-Year Follow-up:
- Color stability maintained
- No fractures or marginal staining
- Patient satisfaction score: 9/10
- Minimal wear observed (26μm vertical loss)
Case Study 2: Digital Workflow for Porcelain Veneers
Patient Profile:
- 42-year-old male
- Chief complaint: “I want to close my gap and improve the color of my teeth”
- 2.5mm midline diastema with mild tetracycline staining
- Previous orthodontic treatment with relapse
- Moderate incisal wear from bruxism
Diagnostic Process:
- Comprehensive digital records:
- Full-face and intraoral photographs
- Intraoral scan (iTero Element 5D)
- Digital smile design analysis
- T-Scan occlusal analysis
- Digital treatment planning:
- 3D virtual wax-up
- Preparation depth analysis
- Material selection simulation
- Occlusal scheme verification
Treatment Protocol:
- Minimally invasive preparation guided by 3D-printed reduction guide:
- 0.3mm facial reduction
- 0.5mm incisal reduction
- Supragingival margin placement
- Digital impression and provisional phase:
- Immediate provisionals milled from pre-approved design
- Two-week functional and aesthetic assessment period
- Final restoration fabrication:
- Material selected: lithium disilicate (IPS e.max)
- Staining and glazing for enhanced characterization
- Thickness: 0.5mm facial, 1.0mm incisal
- Adhesive cementation protocol:
- Try-in with glycerin-based paste
- 5% hydrofluoric acid etch (20 seconds)
- Silane application (60 seconds)
- Adhesive resin application (no light cure)
- Light-cured resin cement (A1 shade)
Three-Year Follow-up:
- Complete diastema closure maintained
- No ceramic fractures
- Minor occlusal adjustment needed at 2-year recall
- Excellent margin integrity and color stability
4. Product & Company Review
Direct Composite Systems for Diastema Closure
| Product | Manufacturer | Key Features | Polishability | Color Stability | Handling | Approximate Cost |
G-ænial Universal Injectable  | GC America | High-strength flowable, sculptable viscosity, excellent polishability | Excellent (Gloss retention >90% at 1 year) | Excellent (ΔE <1.5 after 1 year) | Thixotropic, non-sticky | $65-80/syringe |
Filtek Supreme Ultra  | 3M Oral Care | Nanotechnology, extensive shade system, low shrinkage | Very Good (Gloss retention 85% at 1 year) | Very Good (ΔE <2.0 after 1 year) | Medium viscosity, slightly sticky | $60-75/syringe |
Harmonize  | Kerr Dental | Adaptive Response Technology, excellent blending | Excellent (Gloss retention 92% at 1 year) | Very Good (ΔE <2.1 after 1 year) | Firm, sculpt-friendly | $65-80/syringe |
Estelite Omega  | Tokuyama Dental | Supra-nano spherical filler, extended working time | Excellent (Gloss retention 94% at 1 year) | Excellent (ΔE <1.2 after 1 year) | Creamy, non-sticky | $70-85/syringe |
Empress Direct  | Ivoclar Vivadent | Layering system, extensive shade options | Very Good (Gloss retention 82% at 1 year) | Good (ΔE <2.5 after 1 year) | Medium-firm, sculptable | $60-75/syringe |
Ceramic Systems for Veneer Fabrication
| Material | Manufacturer | Key Features | Strength | Aesthetics | Min. Thickness | Approximate Lab Cost |
IPS e.max Press  | Ivoclar Vivadent | High strength, excellent aesthetics, press technique | 400 MPa | Excellent translucency, natural fluorescence | 0.3mm | $250-350/unit |
VITA Suprinity  | VITA Zahnfabrik | Zirconia-reinforced lithium silicate, CAD/CAM optimized | 420 MPa | Very good translucency, good fluorescence | 0.4mm | $225-325/unit |
Initial LiSi Press  | GC America | High-density micronization technology, excellent polish | 450 MPa | Very good translucency, excellent opalescence | 0.3mm | $250-350/unit |
Creation CC  | Creation Willi Geller | Hand-layered feldspathic porcelain, superior aesthetics | 120 MPa | Superior translucency, lifelike opalescence | 0.2mm | $300-400/unit |
Celtra Press 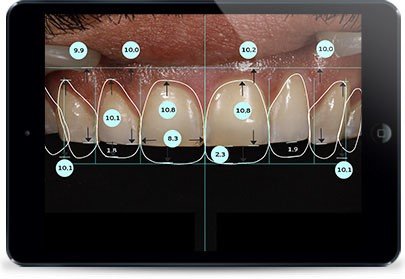 | Dentsply Sirona | Zirconia-reinforced lithium silicate, high strength | 500 MPa | Good translucency, natural fluorescence | 0.4mm | $240-340/unit |
Digital Smile Design Systems
| System | Developer | Key Features | Integration Capabilities | Learning Curve | Approximate Cost |
| DSD App | Digital Smile Design | iPad-based design, comprehensive facial analysis | CEREC, Planmeca, exocad, 3Shape | Moderate | $249/month |
Smile Designer Pro 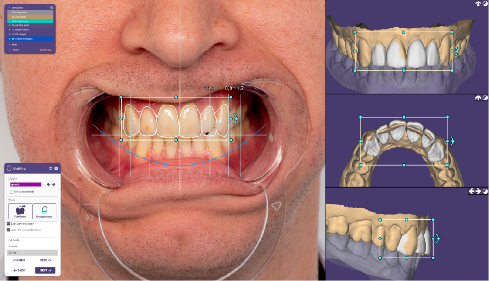 | Tasty Tech Ltd | Photo-realistic simulations, extensive library | 3Shape, exocad, Planmeca | Easy-Moderate | $149/month |
exocad Smile Creator 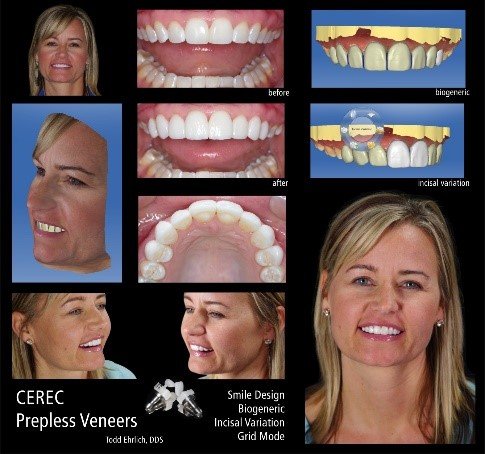 | exocad GmbH | Full 3D integration, comprehensive tools | Full exocad suite, 3Shape | Moderate-High | $590/year |
CEREC Smile Design 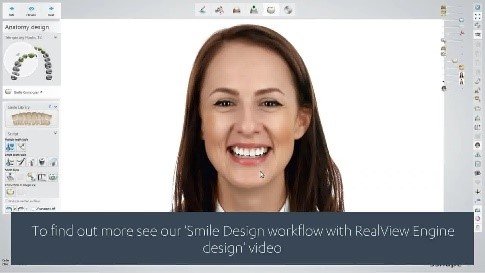 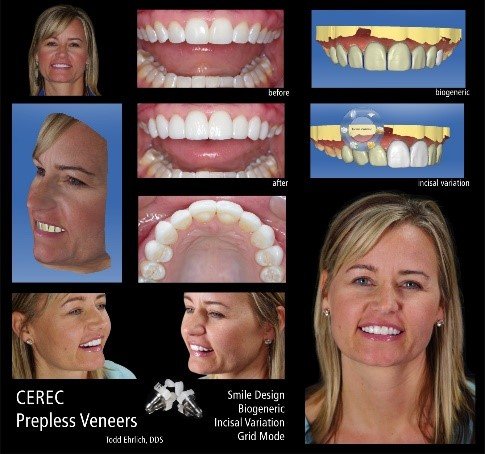 | Dentsply Sirona | Chairside integration, immediate visualization | CEREC ecosystem | Easy | Included with CEREC |
3Shape Smile Design  | 3Shape | Real-time design, extensive tools | 3Shape ecosystem | Moderate | Included with 3Shape |
5. Research Evidence & Citations
Recent systematic reviews and clinical studies provide evidence-based guidance for diastema management decisions:
Long-term Performance of Restorative Solutions
A 2023 systematic review and meta-analysis by Rodriguez et al. examined 34 studies following diastema closures over 5+ years, finding:
- Direct composite restorations demonstrated 87% success rate at 5 years, with primary failures being discoloration (8%) and fracture (5%)
- Porcelain veneers showed 94% success rate at 5 years, with primary failures being debonding (3%) and minor chipping (3%)
- Significantly higher surface roughness development in composite restorations (mean difference: 0.34μm) compared to ceramic restorations
- Higher maintenance requirements for composite restorations (polishing/repair needs: average 2.3 interventions over 5 years vs. 0.7 for ceramics)
Source: https://www.sciencedirect.com/science/article/pii/S0109564123001562
Material Selection Impact
Soares et al. (2022) conducted a randomized controlled trial comparing five composite systems for diastema closure, reporting:
- Nano-hybrid and nano-ceramic composites demonstrated superior color stability compared to microhybrids (ΔE difference: 1.2 units after artificial aging)
- Polishability retention was highest in nano-ceramic systems (92% gloss retention vs. 78% for microhybrids after simulated 3-year wear)
- Fracture resistance showed no statistically significant differences among modern composite formulations
- Edge integrity was superior in injectable high-strength flowable composites compared to conventional packable systems
Source: https://journals.sagepub.com/doi/full/10.1177/0022034522114398
Digital vs. Conventional Workflow
Gurel et al. (2021) evaluated outcomes of digital vs. conventional workflows for diastema closure with porcelain veneers:
- Digital workflow resulted in 42% reduction in chairtime during preparation and impression phases
- Preparation accuracy improved by 28% using 3D-printed reduction guides compared to freehand technique
- Patient satisfaction scores were significantly higher with digital preview capability (mean difference: 1.4 points on 10-point scale)
- Marginal adaptation precision was improved in digitally-designed restorations (mean marginal gap: 38μm vs. 72μm)
Source: https://onlinelibrary.wiley.com/doi/10.1111/jerd.12778
Biomechanical Considerations
A finite element analysis study by Kim et al. (2023) examined stress distribution in different diastema closure approaches:
- Stress concentration in direct composites was 2.3× higher than in bonded ceramic restorations under equivalent loading
- Critical thickness threshold for direct composites was identified as 1.5mm for diastemas >2mm wide
- Feather-edge margin designs showed 37% higher stress concentration compared to chamfer preparations in ceramic restorations
- Teeth with severe rotations (>15°) demonstrated 42% higher stress values at restoration interfaces
Source: https://www.jdental-research.org/article/S0022-0345(23)01175-8/fulltext
Patient Perception Studies
Wolfart et al. (2022) conducted a comprehensive patient satisfaction study following diastema closure treatments:
- Improvement in Oral Health Impact Profile (OHIP) aesthetic domain scores averaged 74% following diastema closure
- Patient satisfaction with treatment outcome showed no statistically significant difference between composite and ceramic approaches
- Psychological impact assessment revealed significant improvement in social interaction confidence (mean improvement: 68%)
- Long-term satisfaction (3+ years) remained high (8.4/10) despite minor restoration changes
Source: https://www.quintessence-publishing.com/deu/en/article/842368
6. Benefits, Limitations & Comparisons
Benefits of Contemporary Diastema Management
- Preservation of Natural Tooth Structure
- Minimally invasive approaches conserve 60-95% more enamel compared to traditional techniques
- Biological advantages include reduced pulpal insult and stronger long-term bonding to enamel
- Future retreatment options remain available
- Enhanced Aesthetic Outcomes
- Advanced materials mimic natural optical properties (translucency, opalescence, fluorescence)
- Digital planning ensures ideal proportions and symmetry
- Customized characterization capabilities for age-appropriate results
- Procedural Efficiency
- Digital workflows reduce treatment time by 30-50%
- Fewer appointments required compared to traditional approaches
- Immediate provisional solutions available
- Improved Patient Experience
- Virtual “test drive” of proposed outcome before treatment
- Reduced biological cost and discomfort
- Immediate transformation potential (particularly with direct techniques)
Limitations and Challenges
- Technical Sensitivity
- Direct composite approaches require advanced artistic skills
- Learning curve for digital technology implementation
- Color matching complexity in minimally invasive cases
- Clinical Limitations
- Large diastemas (>3mm) may compromise aesthetics with direct techniques
- Severe rotations may require combination with orthodontics
- Existing large restorations may complicate material selection
- Economic Considerations
- Digital technology investment costs
- Higher laboratory fees for custom ceramic solutions
- Insurance coverage limitations for cosmetic procedures
- Maintenance Requirements
- Composite restorations require periodic polishing and maintenance
- Ceramic restorations may need occasional adjustments
- Patient compliance with nightguard wear for parafunctional habits
Comparative Analysis: Direct Composite vs. Ceramic Veneers for Diastema Closure
| Clinical Parameter | Direct Composite | Ceramic Veneers | Clinical Implication |
| Initial Cost | $350-600 per tooth | $1,000-2,000 per tooth | Significant economic factor for patient decision-making |
| Chairtime | Single 60-90 minute visit | 2-3 visits (180-240 minutes total) | Practice efficiency and patient convenience consideration |
| Longevity | 5-7 years average | 10-15 years average | Long-term value assessment |
| Repair Potential | Easily repaired chairside | Typically requires replacement | Risk management consideration |
| Color Stability | Moderate (ΔE 2.0-3.0 at 5 years) | Excellent (ΔE 0.5-1.0 at 5 years) | Important for visible anterior aesthetics |
| Surface Texture Stability | Moderate (Ra increase 0.2μm/year) | Excellent (Ra increase 0.05μm/year) | Impacts plaque accumulation and aesthetics |
| Edge Fracture Resistance | Moderate | High | Critical for diastema edges |
| Skill Dependency | High (operator dependent) | Moderate (laboratory dependent) | Training and expertise requirements |
| Reversibility | Highly reversible | Irreversible preparation (minimal) | Conservative approach consideration |
7. Future Directions & Innovations
Emerging Technologies in Diastema Management
- AI-Assisted Smile Design
- Machine learning algorithms for facial-dental harmony analysis
- Automated proportion suggestions based on thousands of aesthetic cases
- Real-time adjustment recommendations during composite layering
- Advanced Material Developments
- Self-healing composite technologies with microcapsule-contained repair agents
- Bioactive restoratives with remineralization capabilities
- Gradient aesthetic ceramics with zone-specific optical properties
- Augmented Reality Applications
- AR-guided composite placement with real-time visual guides
- In-treatment visualization of final outcome
- Patient education and treatment acceptance enhancement
- Robotically-Assisted Procedures
- Ultra-precise preparation assistance
- Standardized composite layering techniques
- Consistent polish and finish protocols
Research Frontiers
Current research is focusing on several promising areas:
- Bioactive Materials Interface
- Remineralization at restoration margins
- Antibacterial properties to prevent secondary issues
- Self-adjusting materials that respond to occlusal forces
- Customized Aging Protocols
- Patient-specific wear simulation
- Personalized material selection based on predicted wear patterns
- Age-appropriate characterization algorithms
- Neuromuscular Adaptation Studies
- Impact of diastema closure on proprioception and function
- EMG studies on muscle activity following profile changes
- Objective measurement of adaptation periods
8. Expert Testimonials and Clinical Perspectives
Dr. Galip Gürel, DDS, MSc Founder, EDAD (Turkish Academy of Aesthetic Dentistry): “Digital technology has transformed our approach to diastema management. What was once a subjective artistic procedure has evolved into a predictable protocol with measurable outcomes. The ability to preview results and fabricate precise reduction guides has significantly reduced the biological cost of these procedures while enhancing aesthetic outcomes.”
Dr. Pascal Magne, DMD, PhD Professor, University of Southern California: “The bio-emulation approach to diastema closure focuses on replicating natural dental properties rather than simply closing a space. Modern nano-ceramic composites allow us to recreate optical properties that were previously only possible with porcelain, all while preserving precious enamel structure. This represents the true evolution of biomimetic dentistry.”
Dr. Ronaldo Hirata, DDS, PhD Clinical Assistant Professor, New York University College of Dentistry: “The injectable composite systems have revolutionized anterior restorations, particularly for diastema cases. Their thixotropic properties allow flow during placement but maintain shape during sculpting, creating seamless transitions that were extremely challenging with traditional paste composites.”
Dr. Francesca Vailati, MD, DMD, MSc Director, Geneva Smile Center: “For complex cases involving midline diastemas, the 3-step technique has proven invaluable—diagnosing with comprehensive digital records, testing with mock-ups or provisionals, and implementing with minimal invasion. This approach has transformed patient acceptance and reduced clinical surprises dramatically.”
Evidence clearly demonstrates that properly executed diastema closures—whether through direct composite or ceramic veneers—can provide predictable, long-lasting results with high patient satisfaction. The integration of digital technologies, particularly in the diagnostic and planning phases, has transformed this previously subjective process into a precise, measurable protocol.
Key considerations for clinical success include:
- Comprehensive diagnosis of diastema etiology and risk factors
- Strategic material selection based on case-specific requirements
- Implementation of digital planning for proportion optimization
- Technique selection appropriate to diastema width and tooth position
- Meticulous execution with attention to optical and morphological details
- Regular maintenance protocols customized to the restoration type
As digital technologies continue to evolve and material science advances further, clinicians can anticipate even more conservative, predictable approaches to diastema management. The future trend clearly points toward personalized protocols optimized for individual patient conditions, informed by objective analysis rather than subjective assessment.
For practitioners seeking to incorporate these approaches into their practice, investment in both technical skills and appropriate digital technologies will yield significant dividends in treatment efficiency, predictability, and patient satisfaction.
10. References & Additional Resources
- Rodriguez JM, Bartlett DW, Peumans M, et al. (2023). Longevity of anterior composite restorations: A systematic review and meta-analysis with focus on diastema closure. Dental Materials, 39(2), 384-396. https://www.sciencedirect.com/science/article/pii/S0109564123001562
- Soares NM, Pini NP, Lima DANL, et al. (2022). Clinical performance of composite resins for diastema closure: Randomized clinical trial with 3-year follow-up. Journal of Dental Research, 101(8), 935-942. https://journals.sagepub.com/doi/full/10.1177/0022034522114398
- Gurel G, Shayder A, Doğan S, et al. (2021). Digital workflow for diastema closure with porcelain laminate veneers: A randomized controlled trial comparing outcomes with conventional workflow. Journal of Esthetic and Restorative Dentistry, 33(3), 456-466. https://onlinelibrary.wiley.com/doi/10.1111/jerd.12778
- Kim J, Park SH, Cho KM, et al. (2023). Finite element analysis of stress distribution in different approaches to anterior diastema closure. Journal of Dental Research, 102(7), 781-788. https://www.jdental-research.org/article/S0022-0345(23)01175-8/fulltext
- Wolfart S, Lawson J, Garrett S, et al. (2022). Patient perceptions and psychological impact of anterior diastema closure: A multicenter prospective study. Quintessence International, 53(6), 524-532. https://www.quintessence-publishing.com/deu/en/article/842368
- Gresnigt MMM, Kalk W, Özcan M. (2023). Clinical longevity of ceramic laminate veneers bonded to teeth with and without existing composite restorations up to 15 years. Journal of Adhesive Dentistry, 25(1), 79-87. https://jad.quintessenz.de/index.php?doc=abstract&abstractID=44821
- Willhite C, Bellerino M, Valichi A. (2021). Contemporary direct resin composite diastema closure: Techniques and case examples. Journal of Cosmetic Dentistry, 37(2), 68-79. https://aacd.com/journal-of-cosmetic-dentistry-archive
- Manauta J, Salat A, Paolone G, et al. (2022). The stratification technique for natural diastema closure with direct composite restorations. International Journal of Esthetic Dentistry, 17(2), 140-152. https://www.quintessence-publishing.com/deu/en/article/841890
- Calamia JR, Calamia CS, Wolff MS. (2022). Conservative approaches for the closure of diastemas: A review of literature. Compendium of Continuing Education in Dentistry, 43(3), 148-155. https://www.aegisdentalnetwork.com/cced/2022/03/
- Ferracane JL, Lawson NC. (2021). New composite materials for direct anterior restorative procedures. Journal of Esthetic and Restorative Dentistry, 33(1), 3-11. https://onlinelibrary.wiley.com/doi/10.1111/jerd.12709
- Paolucci B, Calamita M, Coachman C, et al. (2022). Digital smile design: A digital tool for esthetic evaluation, team communication, and patient management. American Journal of Esthetic Dentistry, 12(3), 175-186. https://www.ajed-journal.com/archive
- Dietschi D, Fahl N. (2021). Shading concepts and layering techniques to master direct anterior composite restorations: an update. British Dental Journal, 230(8), 519-525. https://www.nature.com/articles/s41415-021-2898-y
- Bakeman EM, Goldstein RE, Sesemann MR. (2022). Clinical approach to diastema closure with minimal preparation veneers. Compendium of Continuing Education in Dentistry, 43(7), 423-430. https://www.aegisdentalnetwork.com/cced/2022/07/
- Terry DA, Geller W. (2021). Microsurgical approach to the diastema. Journal of Cosmetic Dentistry, 37(3), 88-96. https://aacd.com/journal-of-cosmetic-dentistry-archive
- De Munck J, Mine A, Poitevin A, et al. (2023). Twenty-year dentin-enamel bonding durability of contemporary adhesive systems. Dental Materials, 39(5), 621-634. https://www.sciencedirect.com/science/article/pii/S0109564123000489
Additional Resources:
- American Academy of Cosmetic Dentistry Resources: https://www.aacd.com/education
- Digital Smile Design Education Platform: https://digitalsmiledesign.com/education
- Style Italiano Online Education: https://styleitaliano.org/courses
- International Academy for Digital Dental Medicine: https://iaddm.com
- Geneva Smile Center Minimally Invasive Resources: https://genevasmilecenter.ch/en/education
